Sodium-Glucose Cotransporter-2 Inhibitors in Critically Ill Patients and Acute Kidney Injury: Clinical Considerations
Main Article Content
Abstract
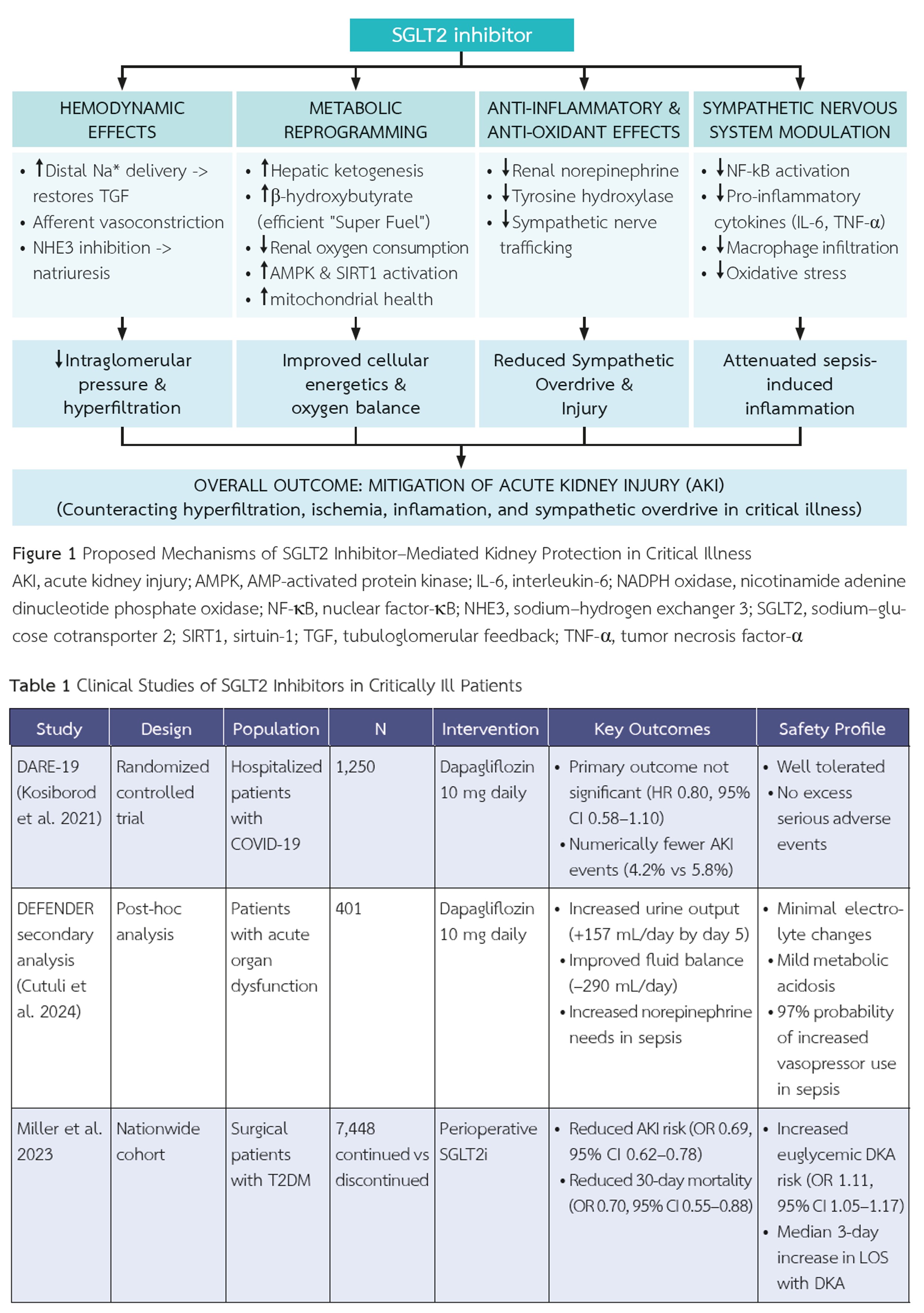
Acute kidney injury (AKI) is a severe complication, affecting up to 50% of critically ill patients. The advent of sodium-glucose cotransporter-2 (SGLT2) inhibitors has challenged traditional paradigms of renoprotection. Their mechanisms include restoration of tubuloglomerular feedback, metabolic reprogramming toward ketone utilization, anti-inflammatory actions, and modulation of the sympathetic nervous system. Emerging evidence suggests a complex risk–benefit profile for SGLT2 inhibitors in critical illness. Observational studies consistently show associations with reduced ICU admissions, lower infection rates, and improved survival. However, interventional studies indicate nuanced effects, including potential increases in vasopressor requirements in septic patients. The ongoing PREVENTS-AKI trial, specifically designed for ICU patients, will provide definitive evidence to guide clinical practice. The use of SGLT2 inhibitors in this vulnerable population requires careful consideration of unique safety concerns, including euglycemic diabetic ketoacidosis, increased vasopressor requirements, electrolyte disturbances, volume depletion, and genitourinary infections. Implementation should follow structured protocols with a thorough baseline assessment, daily monitoring, and clear discontinuation criteria. Until more robust evidence emerges, SGLT2 inhibitors represent a promising but cautiously applied option for AKI prevention in selected critically ill patients.
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
This article is published under CC BY-NC-ND 4.0 license, which allows for non-commercial reuse of the published paper as long as the published paper is fully attributed. Anyone can share (copy and redistribute) the material in any medium or format without having to ask permission from the author or the Nephrology Society of Thailand.
References
Hoste EA, Bagshaw SM, Bellomo R, Cely CM, Colman R, Cruz DN, et al. Epidemiology of acute kidney injury in critically ill patients: the multinational AKI-EPI study. Intensive Care Med 2015;41(8):1411–23. doi: 10.1007/s00134-015-3934-7.
Uchino S, Kellum JA, Bellomo R, Doig GS, Morimatsu H, Morgera S, et al. Acute renal failure in critically ill patients: a multinational, multicenter study. JAMA 2005;294(7):813–8. doi: 10.1001/jama.294.7.813.
Peerapornratana S, Manrique-Caballero CL, Gomez H, Kellum JA. Acute kidney injury from sepsis: current concepts, epidemiology, pathophysiology, prevention and treatment. Kidney Int 2019;96(5):1083–99. doi: 10.1016/j.kint.2019.05.026.
Pickkers P, Darmon M, Hoste E, Joannidis M, Legrand M, Ostermann M, et al. Acute kidney injury in the critically ill: an updated review on pathophysiology and management. Intensive Care Med 2021;47(8):835–50. doi: 10.1007/s00134-021-06454-7.
DeFronzo RA, Norton L, Abdul-Ghani M. Renal, metabolic and cardiovascular considerations of SGLT2 inhibition. Nat Rev Nephrol 2017;13(1):11–26. doi: 10.1038/nrneph.2016.170.
Zinman B, Wanner C, Lachin JM, Fitchett D, Bluhmki E, Hantel S, et al. Empagliflozin, Cardiovascular Outcomes, and Mortality in Type 2 Diabetes. N Engl J Med 2015;373(22):2117–28. doi:10.1056/NEJMoa1504720.
Neal B, Perkovic V, Mahaffey KW, de Zeeuw D, Fulcher G, Erondu N, et al. Canagliflozin and Cardiovascular and Renal Events in Type 2 Diabetes. N Engl J Med 2017;377(7):644–57. doi: 10.1056/NEJMoa1611925.
Wiviott SD, Raz I, Bonaca MP, Mosenzon O, Kato ET, Cahn A, et al. Dapagliflozin and Cardiovascular Outcomes in Type 2 Diabetes. N Engl J Med 2019;380(4):347–57. doi: 10.1056/NEJMoa1812389.
Perkovic V, Jardine MJ, Neal B, Bompoint S, Heerspink HJL, Charytan DM, et al. Canagliflozin and Renal Outcomes in Type 2 Diabetes and Nephropathy. N Engl J Med 2019;380(24):2295–306. doi: 10.1056/NEJMoa1811744.
Heerspink HJL, Stefansson BV, Correa-Rotter R, Chertow GM, Greene T, Hou FF, et al. Dapagliflozin in Patients with Chronic Kidney Disease. N Engl J Med 2020;383(15):1436–46. doi:10.1056/NEJMoa2024816.
The E-KCG, Herrington WG, Staplin N, Wanner C, Green JB, Hauske SJ, et al. Empagliflozin in Patients with Chronic Kidney Disease. N Engl J Med 2023;388(2):117–27. doi: 10.1056/NEJMoa2204233.
Kidney Disease: Improving Global Outcomes Diabetes Work G. KDIGO 2022 Clinical Practice Guideline for Diabetes Management in Chronic Kidney Disease. Kidney Int 2022;102(5S):S1–S127. doi: 10.1016/j.kint.2022.06.008.
Vallon V, Thomson SC. The tubular hypothesis of nephron filtration and diabetic kidney disease. Nat Rev Nephrol 2020;16(6):317–36. doi: 10.1038/s41581-020-0256-y.
Thomson SC, Rieg T, Miracle C, Mansoury H, Whaley J, Vallon V, et al. Acute and chronic effects of SGLT2 blockade on glomerular and tubular function in the early diabetic rat. Am J Physiol Regul Integr Comp Physiol 2012;302(1):R75–83. doi: 10.1152/ajpregu.00357.2011.
Cherney DZ, Perkins BA, Soleymanlou N, Maione M, Lai V, Lee A, et al. Renal hemodynamic effect of sodium-glucose cotransporter 2 inhibition in patients with type 1 diabetes mellitus. Circulation 2014;129(5):587–97. doi: 10.1161/CIRCULATIONAHA.113.005081.
van Bommel EJM, Muskiet MHA, van Baar MJB, Tonneijck L, Smits MM, Emanuel AL, et al. The renal hemodynamic effects of the SGLT2 inhibitor dapagliflozin are caused by post-glomerular vasodilatation rather than pre-glomerular vasoconstriction in metformin-treated patients with type 2 diabetes in the randomized, double-blind RED trial. Kidney Int 2020;97(1):202–12. doi:10.1016/j.kint.2019.09.013.
Onishi A, Fu Y, Patel R, Darshi M, Crespo-Masip M, Huang W, et al. A role for tubular Na(+)/H(+) exchanger NHE3 in the natriuretic effect of the SGLT2 inhibitor empagliflozin. Am J Physiol Renal Physiol 2020;319(4):F712–F28. doi: 10.1152/ajprenal.00264.2020.
Hallow KM, Helmlinger G, Greasley PJ, McMurray JJV, Boulton DW. Why do SGLT2 inhibitors reduce heart failure hospitalization? A differential volume regulation hypothesis. Diabetes Obes Metab 2018;20(3):479–87. doi:10.1111/dom.13126.
Ferrannini E, Mark M, Mayoux E. CV Protection in the EMPA-REG OUTCOME Trial: A “Thrifty Substrate” Hypothesis. Diabetes Care 2016;39(7):1108–14. doi: 10.2337/dc16-0330.
Mudaliar S, Alloju S, Henry RR. Can a Shift in Fuel Energetics Explain the Beneficial Cardiorenal Outcomes in the EMPA-REG OUTCOME Study? A Unifying Hypothesis. Diabetes Care 2016;39(7):1115–22. doi: 10.2337/dc16-0542.
Zanchi A, Burnier M, Muller ME, Ghajarzadeh-Wurzner A, Maillard M, Loncle N, et al. Acute and Chronic Effects of SGLT2 Inhibitor Empagliflozin on Renal Oxygenation and Blood Pressure Control in Nondiabetic Normotensive Subjects: A Randomized, Placebo-Controlled Trial. J Am Heart Assoc 2020;9(13):e016173. doi: 10.1161/JAHA.119.016173.
Hawley SA, Ford RJ, Smith BK, Gowans GJ, Mancini SJ, Pitt RD, et al. The Na+/Glucose Cotransporter Inhibitor Canagliflozin Activates AMPK by Inhibiting Mitochondrial Function and Increasing Cellular AMP Levels. Diabetes 2016;65(9):2784–94. doi: 10.2337/db16-0058.
Packer M. Critical Reanalysis of the Mechanisms Underlying the Cardiorenal Benefits of SGLT2 Inhibitors and Reaffirmation of the Nutrient Deprivation Signaling/Autophagy Hypothesis. Circulation 2022;146(18):1383–405. doi: 10.1161/CIRCULATIONAHA. 122.061732.
Heerspink HJL, Perco P, Mulder S, Leierer J, Hansen MK, Heinzel A, et al. Canagliflozin reduces inflammation and fibrosis biomarkers: a potential mechanism of action for beneficial effects of SGLT2 inhibitors in diabetic kidney disease. Diabetologia 2019;62(7):1154–66. doi: 10.1007/s00125-019-4859-4.
Dekkers CCJ, Petrykiv S, Laverman GD, Cherney DZ, Gansevoort RT, Heerspink HJL. Effects of the SGLT-2 inhibitor dapagliflozin on glomerular and tubular injury markers. Diabetes Obes Metab 2018;20(8):1988–93. doi: 10.1111/dom.13301.
Au PCM, Tan KCB, Cheung BMY, Wong ICK, Wong Y, Cheung CL. Association Between SGLT2 Inhibitors vs DPP-4 Inhibitors and Risk of Pneumonia Among Patients With Type 2 Diabetes. J Clin Endocrinol Metab 2022;107(4):e1719–e26. doi: 10.1210/clinem/dgab818.
Li CY, Wang LX, Dong SS, Hong Y, Zhou XH, Zheng WW, et al. Phlorizin Exerts Direct Protective Effects on Palmitic Acid (PA)-Induced Endothelial Dysfunction by Activating the PI3K/AKT/eNOS Signaling Pathway and Increasing the Levels of Nitric Oxide (NO). Med Sci Monit Basic Res 2018;24:1–9. doi:10.12659/msmbr.907775.
Matthews VB, Elliot RH, Rudnicka C, Hricova J, Herat L, Schlaich MP. Role of the sympathetic nervous system in regulation of the sodium glucose cotransporter 2. J Hypertens 2017;35(10):2059–68. doi: 10.1097/HJH.0000000000001434.
Herat LY, Magno AL, Rudnicka C, Hricova J, Carnagarin R, Ward NC, et al. SGLT2 Inhibitor-Induced Sympathoinhibition: A Novel Mechanism for Cardiorenal Protection. JACC Basic Transl Sci 2020;5(2):169–79. doi: 10.1016/j.jacbts.2019.11.007.
Sano M. A new class of drugs for heart failure: SGLT2 inhibitors reduce sympathetic overactivity. J Cardiol 2018;71(5):471–6. doi:10.1016/j.jjcc.2017.12.004.
Ng PY, Ng AK, Ip A, Wu MZ, Guo R, Yiu KH. Risk of ICU Admission and Related Mortality in Patients With Sodium-Glucose Cotransporter 2 Inhibitors and Dipeptidyl Peptidase-4 Inhibitors: A Territory-Wide Retrospective Cohort Study. Crit Care Med 2023;51(8):1074–85. doi: 10.1097/CCM.0000000000005869.
Wu MZ, Chandramouli C, Wong PF, Chan YH, Li HL, Yu SY, et al. Risk of sepsis and pneumonia in patients initiated on SGLT2 inhibitors and DPP-4 inhibitors. Diabetes Metab 2022;48(6):101367. doi: 10.1016/j.diabet.2022.101367.
Ashcherkin N, Abdalla AA, Gupta S, Bhatt S, Yee CI, Cartin-Ceba R. Are sodium-glucose co-transporter-2 inhibitors associated with improved outcomes in diabetic patients admitted to intensive care units with septic shock? Acute Crit Care 2024;39(2):251–6. doi:10.4266/acc.2023.01046.
Singh LG, Ntelis S, Siddiqui T, Seliger SL, Sorkin JD, Spanakis EK. Association of Continued Use of SGLT2 Inhibitors From the Ambulatory to Inpatient Setting With Hospital Outcomes in Patients With Diabetes: A Nationwide Cohort Study. Diabetes Care 2024;47(6):933–40. doi: 10.2337/dc23-1129.
Martensson J, Cutuli SL, Osawa EA, Yanase F, Toh L, Cioccari L, et al. Sodium glucose co-transporter-2 inhibitors in intensive care unit patients with type 2 diabetes: a pilot case control study. Crit Care 2023;27(1):189. doi: 10.1186/s13054-023-04481-y.
Kosiborod MN, Esterline R, Furtado RHM, Oscarsson J, Gasparyan SB, Koch GG, et al. Dapagliflozin in patients with cardiometabolic risk factors hospitalised with COVID-19 (DARE-19): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Diabetes Endocrinol 2021;9(9):586–94. doi: 10.1016/S2213-8587(21)00180-7.
Zampieri FG, Azevedo LCP, Neto AS, Rea-Neto A, David-Joao PG, Amendola CP, et al. Effects of dapagliflozin on urinary output, fluid balance, and biochemistry in critically ill patients: a post-hoc secondary analysis of the DEFENDER trial. Crit Care 2025;29(1):297. doi:10.1186/s13054-025-05534-0.
Tallarico RT, Jing B, Lu K, Chawla SA, Luo Y, Badathala A, et al. Postoperative Outcomes Among Sodium-Glucose Cotransporter 2 Inhibitor Users. JAMA Surg 2025;160(6):681–9. doi: 10.1001/jamasurg.2025.0940.
Butler J, Jones WS, Udell JA, Anker SD, Petrie MC, Harrington J, et al. Empagliflozin after Acute Myocardial Infarction. N Engl J Med 2024;390(16):1455–66. doi: 10.1056/NEJMoa2314051.
Voors AA, Angermann CE, Teerlink JR, Collins SP, Kosiborod M, Biegus J, et al. The SGLT2 inhibitor empagliflozin in patients hospitalized for acute heart failure: a multinational randomized trial. Nat Med 2022;28(3):568–74. doi: 10.1038/s41591-021-01659-1.
Bhatt DL, Szarek M, Steg PG, Cannon CP, Leiter LA, McGuire DK, et al. Sotagliflozin in Patients with Diabetes and Recent Worsening Heart Failure. N Engl J Med 2021;384(2):117–28. doi: 10.1056/NEJMoa2030183.
Goldenberg RM, Berard LD, Cheng AYY, Gilbert JD, Verma S, Woo VC, et al. SGLT2 Inhibitor-associated Diabetic Ketoacidosis: Clinical Review and Recommendations for Prevention and Diagnosis. Clin Ther 2016;38(12):2654–64 e1. doi: 10.1016/j.clinthera.2016.11.002.
Blau JE, Tella SH, Taylor SI, Rother KI. Ketoacidosis associated with SGLT2 inhibitor treatment: Analysis of FAERS data. Diabetes Metab Res Rev 2017;33(8). doi: 10.1002/dmrr.2924.
Ferrannini E, Muscelli E, Frascerra S, Baldi S, Mari A, Heise T, et al. Metabolic response to sodium-glucose cotransporter 2 inhibition in type 2 diabetic patients. J Clin Invest 2014;124(2):499–508. doi: 10.1172/JCI72227.
Sanusi I, Sarnowski A, Russell-Jones D, Forni LG. A potential diagnostic problem on the ICU: Euglycaemic diabetic Ketoacidosis associated with SGLT2 inhibition. J Crit Care 2020;57:19–22. doi: 10.1016/j.jcrc.2019.12.007.
Savage MW, Dhatariya KK, Kilvert A, Rayman G, Rees JA, Courtney CH, et al. Joint British Diabetes Societies guideline for the management of diabetic ketoacidosis. Diabet Med 2011;28(5):508–15. doi: 10.1111/j.1464-5491.2011.03246.x.
Thiruvenkatarajan V, Meyer EJ, Nanjappa N, Van Wijk RM, Jesudason D. Perioperative diabetic ketoacidosis associated with sodium-glucose co-transporter-2 inhibitors: a systematic review. Br J Anaesth 2019;123(1):27–36. doi: 10.1016/j.bja.2019.03.028.
Darmon M, Timsit JF, Francais A, Nguile-Makao M, Adrie C, Cohen Y, et al. Association between hypernatraemia acquired in the ICU and mortality: a cohort study. Nephrol Dial Transplant 2010;25(8):2510–5. doi: 10.1093/ndt/gfq067.
Packer M, Wilcox CS, Testani JM. Critical Analysis of the Effects of SGLT2 Inhibitors on Renal Tubular Sodium, Water and Chloride Homeostasis and Their Role in Influencing Heart Failure Outcomes. Circulation 2023;148(4):354–72. doi:10.1161/CIRCULATIONAHA.123.064346.
Menne J, Dumann E, Haller H, Schmidt BMW. Acute kidney injury and adverse renal events in patients receiving SGLT2-inhibitors: A systematic review and meta-analysis. PLoS Med 2019;16(12):e1002983. doi: 10.1371/journal.pmed.1002983.
Kraus BJ, Weir MR, Bakris GL, Mattheus M, Cherney DZI, Sattar N, et al. Characterization and implications of the initial estimated glomerular filtration rate ‘dip’ upon sodium-glucose cotransporter-2 inhibition with empagliflozin in the EMPA-REG OUTCOME trial. Kidney Int 2021;99(3):750–62. doi: 10.1016/j.kint.2020.10.031.
Puckrin R, Saltiel MP, Reynier P, Azoulay L, Yu OHY, Filion KB. SGLT-2 inhibitors and the risk of infections: a systematic review and meta-analysis of randomized controlled trials. Acta Diabetol 2018;55(5):503–14. doi: 10.1007/s00592-018-1116-0.
ClinicalTrials.gov. PREVENTion with Sglt2 inhibition of Acute Kidney Injury in intensive care (PREVENTS-AKI). NCT05468203. Available from: https://clinicaltrials.gov/ct2/show/NCT05468203. Accessed December 15, 2024.
ClinicalTrials.gov. SGLT2 Inhibitor Treatment After Acute Kidney Injury. NCT05360615. Available from: https://clinicaltrials.gov/ct2/show/NCT05360615. Accessed December 15, 2024.
ClinicalTrials.gov. A Study to Evaluate the Effect of Dapagliflozin on Renal and Cardiovascular Outcomes in Patients With Advanced CKD (RENAL LIFECYCLES). NCT05374291. Available from: https://clinicaltrials.gov/ct2/show/NCT05374291. Accessed December 15, 2024.