Clinical Application of Bioelectrical Impedance Analysis for Fluid Assessment in Hemodialysis Patients
Main Article Content
Abstract
Background: Fluid overload is common in maintenance hemodialysis (MHD) patients and is associated with adverse cardiovascular events and mortality. Conventional clinical methods for fluid assessment have limited accuracy. This study evaluated the effectiveness of bioelectrical impedance analysis (BIA) for the fluid evaluation in MHD patients.
Methods: A prospective interventional study was conducted in 34 clinically stable MHD patients at Ranong Hospital from June to August 2025. Fluid status was assessed monthly using BIA, combined with standard of care, and dry body weight was adjusted accordingly. The outcomes were the change in fluid status, expressed as target average fluid overload (TAFO), dialysis-related complications, and blood pressure control before and after BIA-guided management.
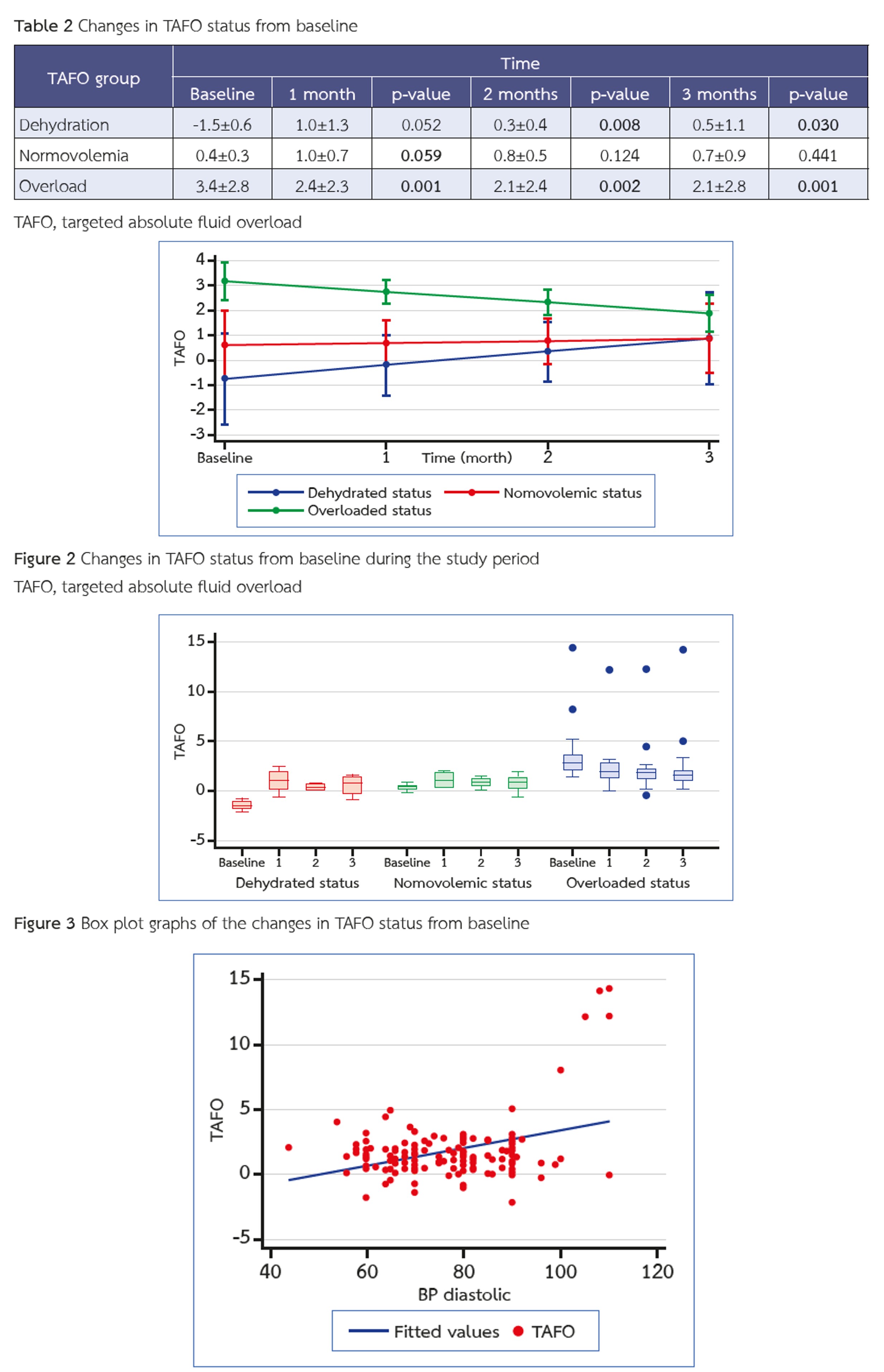
Results: At baseline, 67.6% of patients were fluid overloaded, 20.6% were normovolemic, and 11.8% were dehydrated. In the overloaded group, mean TAFO significantly decreased from 3.4 ± 2.8 L to 2.1 ± 2.8 L at 3 months (p = 0.001). Dehydrated patients shifted toward normovolemia, while normovolemic patients remained stable. Dialysis-related complications, including intradialytic hypotension and hypertension, symptoms of cramps and fatigue, improved significantly in the overload group. The mean number of antihypertensive drug classes was also substantially reduced.
Conclusions: BIA-guided fluid management improved fluid control in MHD patients, resulting in reduced dialysis-related complications and fewer anti-hypertensive drug classes. These findings support integrating BIA into standard clinical practice for individualized volume management, particularly in patients with fluid overload.
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
This article is published under CC BY-NC-ND 4.0 license, which allows for non-commercial reuse of the published paper as long as the published paper is fully attributed. Anyone can share (copy and redistribute) the material in any medium or format without having to ask permission from the author or the Nephrology Society of Thailand.
References
Moissl U, Arias-Guillen M, Wabel P, Fontsere N, Carrera M, Campistol JM, et al. Bioimpedance-guided fluid management in hemodialysis patients. Clin J Am Soc Nephrol 2013;8(9):1575–82. doi: 10.2215/CJN.12411212.
Antlanger M, Hecking M, Haidinger M, Werzowa J, Kovarik JJ, Paul G, et al. Fluid overload in hemodialysis patients: a cross-sectional study to determine its association with cardiac biomarkers and nutritional status. BMC Nephrol 2013;14:266. doi: 10.1186/1471-2369-14-266.
Dekker MJ, Marcelli D, Canaud BJ, Carioni P, Wang Y, Grassmann A, et al. Impact of fluid status and inflammation and their interaction on survival: a study in an international hemodialysis patient cohort. Kidney Int 2017;91(5):1214–23. doi: 10.1016/j.kint.2016.12.008.
Cheng L, Chang L, Tian R, Zhou J, Luo F, Zhang H. The predictive value of bioimpedance-derived fluid parameters for cardiovascular events in patients undergoing hemodialysis. Ren Fail 2022;44(1):1192–200. doi: 10.1080/0886022X.2022.2095287.
Flythe JE, Chang TI, Gallagher MP, Lindley E, Madero M, Sarafidis PA, et al. Blood pressure and volume management in dialysis: conclusions from a Kidney Disease: Improving Global Outcomes (KDIGO) Controversies Conference. Kidney Int 2020;97(5):861–76. doi: 10.1016/j.kint.2020.01.046.
Davies SJ, Davenport A. The role of bioimpedance and biomarkers in helping to aid clinical decision-making of volume assessments in dialysis patients. Kidney Int 2014;86(3):489–96. doi: 10.1038/ki.2014.207.
Eyre S, Stenberg J, Wallengren O, Keane D, Avesani CM, Bosaeus I, et al. Bioimpedance analysis in patients with chronic kidney disease. Wiley Online Library; 2023. p. 147–57.
Ophascharoensuk V, Peerapornratana S. Executive Summary of the 2022 Thailand Hemodialysis Clinical Practice Guideline. Journal of the Nephrology Society of Thailand 2023;29(4):289–300.
Agarwal R, Alborzi P, Satyan S, Light RP. Dry-weight reduction in hypertensive hemodialysis patients (DRIP): a randomized, controlled trial. Hypertension 2009;53(3):500–7. doi: 10.1161/HYPERTENSIONAHA.108.125674.
Covic A, Ciumanghel A-I, Siriopol D, Kanbay M, Dumea R, Gavrilovici C, et al. Value of bioimpedance analysis estimated “dry weight” in maintenance dialysis patients: a systematic review and meta-analysis. Int urol nephrol 2017;49:2231–45. doi: 10.1007/s11255-017-1698-4
Hur E, Usta M, Toz H, Asci G, Wabel P, Kahvecioglu S, et al. Effect of fluid management guided by bioimpedance spectroscopy on cardiovascular parameters in hemodialysis patients: a randomized controlled trial. Am J Kidney Dis 2013;61(6):957–65. doi: 10.1053/j.ajkd.2012.12.017.