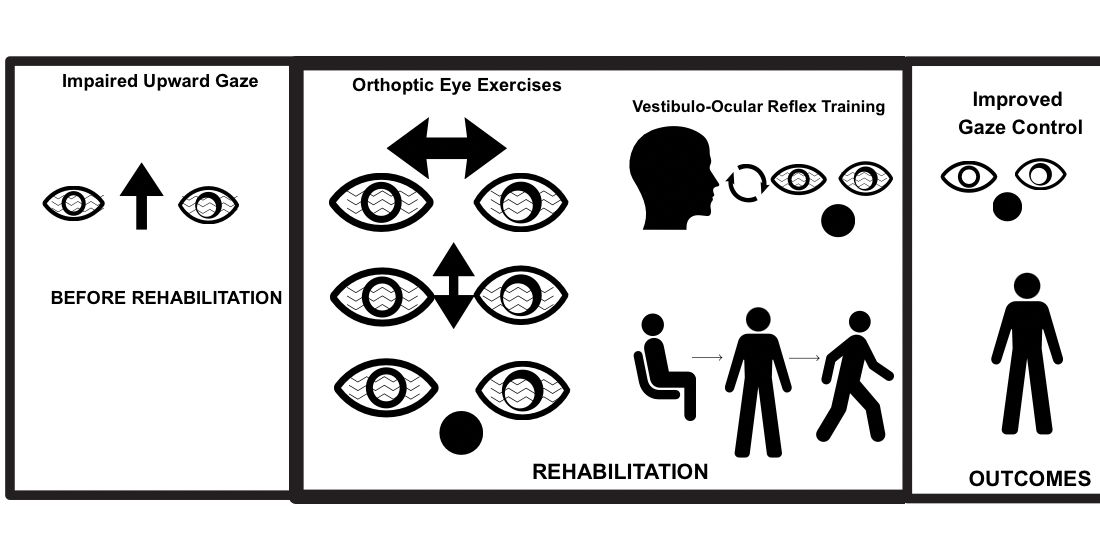
Visual-Vestibular Rehabilitation Using Orthoptic and Vestibulo-Ocular Reflex Training in Parinaud Syndrome: A Case Report
Keywords:
midbrain syndrome, orthoptic exercises, stroke, health and wellbeing, quality of lifeAbstract
Parinaud syndrome, or dorsal midbrain syndrome, is a rare neuro-ophthalmological disorder characterized by vertical gaze palsy, convergence-retraction nystagmus, light-near dissociation, and impaired convergence. Rehabilitation literature has primarily focused on motor outcomes in stroke, with limited evidence on visual rehabilitation in this Syndrome. A 39-year-old female presented with acute thalamic-midbrain hemorrhage and developed Parinaud Syndrome with vertical gaze palsy, convergence-retraction nystagmus, diplopia, and impaired near point of convergence. A structured visual-vestibular rehabilitation protocol was implemented, consisting of orthoptic training (pencil push-ups, stereogram fusion, saccadic tracking, smooth pursuits) and vestibulo-ocular reflex (VOR) training (gaze stabilization drills). The program was delivered for 4 weeks, 5 sessions per week. The patient showed partial restoration of upward gaze, improved convergence, reduced diplopia, and enhanced gaze stability. Near point of convergence improved, facilitating better reading ability and daily visual tasks with less fatigue. Functionally, she reported greater independence and confidence in activities requiring visual control. This case demonstrates the effectiveness of targeted visual-vestibular rehabilitation in Parinaud Syndrome, highlighting the role of orthoptic and vestibulo-ocular reflex exercises in improving ocular motility and functional vision. Future studies exploring digital eye-tracking and virtual reality may further enhance rehabilitation outcomes in this rare condition.
References
Miller NR, Newman NJ. Walsh & Hoyt’s clinical neuro-ophthalmology. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2005.
Asirvatham T, Boppana A, Chandran PI, Jamaludeen SA. Innovative rehabilitation intervention in a young stroke patient with Parinaud syndrome: a case report. Qatar Med J. 2025;2025:30. PubMed PMID: 40454414
Savitz SI, Baron JC, Fisher M. Stroke and midbrain involvement: clinical and radiologic characteristics. Stroke. 2019;50:713-20.
Sheikh SI, Ghassemi P, Zhao H. Vestibulo-ocular rehabilitation after brain injury: clinical evidence and application. Front Neurol. 2021;12:622031.
Porciatti V, Wong AMF, Lennerstrand G. Orthoptic therapy for visual dysfunctions in neurologic conditions: a narrative review. Neuroophthalmology. 2022; 46:34-42.
Siva S, Elambirainathan S, Ramesh S, Sridharan P. Effectiveness of orthoptic exercises for symptomatic convergence insufficiency in post-stroke patients: a single case study. Texila Int J Public Health. 2025.
Fetter M. Vestibulo-ocular reflex. Dev Ophthalmol. 2007;40:35-51.
Herdman SJ, Clendaniel RA. Vestibular rehabilitation. 4th ed. Philadelphia: F.A. Davis Company; 2020.
Sathiyaseelan N, Subramanian SS, Kumaresan A, Vishuram S, Gayathri KC, Sekar M, et al. Effectiveness of biopsychosocial approach for subacute neck pain among geriatrics. Fizjoterapia Pol. 2024;24:147-52.
Chen CC, Heinemann AW, Bode RK, Granger CV, Mallinson T. Impact of visual field deficits on functional outcomes in stroke rehabilitation. Am J Phys Med Rehabil. 2007;86:665-72.
Unnikrishnan R, Alagesan J, Alzhrani M, Alanazi A, Sirajudeen MS, Ateef M et al. Relationship between Kinesthesia and Motor Performance in Young Adults with Generalized Joint Hypermobility: A Systematic Review. Journal of Pharmacy and Bioallied Sciences. 2024;16(Suppl_4):S3056-9.