Association Between Polypharmacy and Frailty in Elderly Patients Receiving Care at a Public Hospital in South India
Keywords:
elderly, frailty, polypharmacy, Tilburg Frailty Indicator, prevalenceAbstract
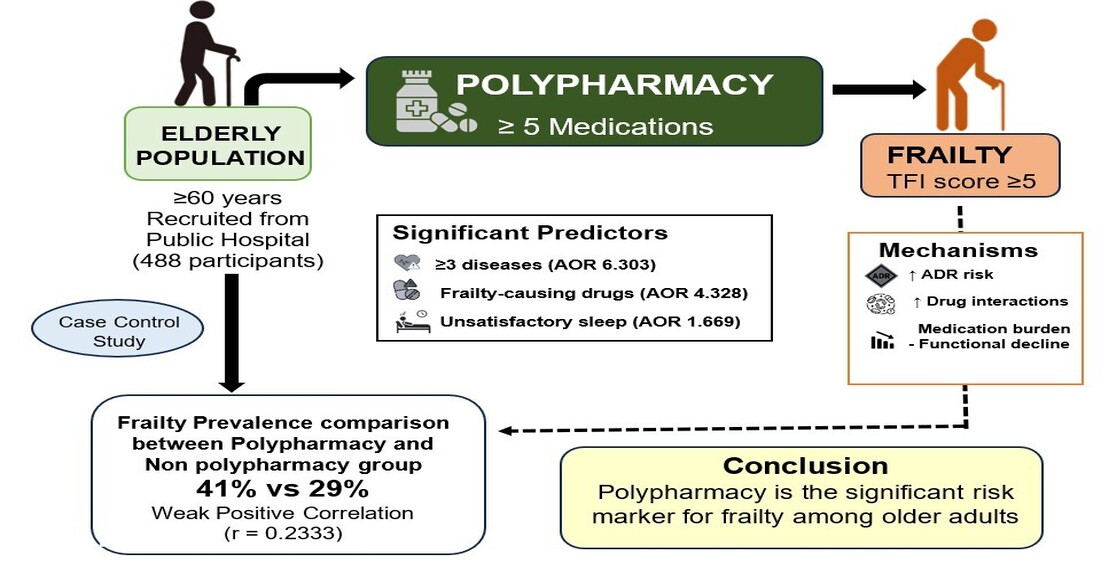
Objective This study analyses the impact of polypharmacy on frailty among the elderly patients visiting the public sector hospitals. The present study was done to assess the frailty status of the elderly patients and to see whether the individuals with polypharmacy exhibited more frailty when compared to those without polypharmacy.
Methods This is a case-control study that included 488 participants age 60 years and above who visited the general medicine department of Public Hospital Ooty, India. Polypharmacy was defined as the concomitant use of 5 or more medications. Frailty status of the participants was assessed using the Tilburg Frailty Indicator.
Results Polypharmacy was found to be present in 34.42% of cases. The prevalence of frailty was significantly higher in the polypharmacy group, affecting 41.07% of the study participants. Finally, three variables emerged as influential predictors of polypharmacy namely, 3 or more diseases (AOR 6.303, Cl 4.009-9.911, p < 0.0001), unsatisfied sleep status (AOR 1.669, Cl 1.068-2.606, p = 0.01), and people taking frailty causing drugs (AOR 4.328, Cl 2.628-7.128, p = 0.003). Additionally, there was a moderate relationship between modified lifestyle (smoking, alcohol consumption) and polypharmacy.
Conclusions The results suggest that polypharmacy is linked with frailty among the elderly population, highlighting the importance of clinician awareness of these factors.
References
Mohammad G, Singh S, Singh P, Gautam V, Pillai VA. Analysis of the prevalence and pattern of polypharmacy among elderly patients admitted in general medicine department of a rural tertiary care hospital in south India. Asian Journal of Medical Sciences. 2023;14:146-50.
Srijayanth K, Maiya RG. Quality of life among geriatric population: A cross-sectional study to assess the quality of life among geriatric population covered under urban health training center of a tertiary care hospital in Kancheepuram, Tamilnadu. Indian J Prev Soc Med. 2022;53:199-205.
Dagli RJ, Sharma A. Polypharmacy: a global risk factor for elderly people. J Int Oral Health. 2014;6:i-ii. PubMed PMID: 25628499.
World Health Organization. Medication safety in polypharmacy: a WHO technical report. Geneva: World Health Organization; 2019.
Ahmed N, Mandel R, Fain MJ. Frailty: an emerging geriatric syndrome. The American journal of medicine. 2007;120:748-53.
Veronese N, Stubbs B, Noale M, Solmi M, Pilotto A, Vaona A, et al. Polypharmacy is associated with higher frailty risk in older people: an 8-year longitudinal cohort study. J Am Med Dir Assoc. 2017;18:624-8.
Coelho T, Paúl C, Gobbens RJ, Fernandes L. Determinants of frailty: the added value of assessing medication. Front Aging Neurosci. 2015;7:56. PubMed PMID: 25954195.
Nishtala PS, Narayan SW, Wang T, Hilmer SN. Associations of drug burden index with falls, general practitioner visits, and mortality in older people. Pharmacoepidemiol Drug Saf. 2014;23:753-8.
Jyrkkä J, Enlund H, Korhonen MJ, Sulkava R, Hartikainen S. Polypharmacy status as an indicator of mortality in an elderly population. Drugs Aging. 2009;26: 1039-48.
Herr M, Robine JM, Pinot J, Arvieu JJ, Ankri J. Polypharmacy and frailty: prevalence, relationship, and impact on mortality in a French sample of 2350 old people. Pharmacoepidemiol Drug Saf. 2015;24:637-46.
Gutiérrez-Valencia M, Izquierdo M, Cesari M, Casas-Herrero Á, Inzitari M, Martínez-Velilla N. The relationship between frailty and polypharmacy in older people: a systematic review. Br J Clin Pharmacol. 2018;84:1432-44.
Bhagavathula AS, Vidyasagar K, Chhabra M, Rashid M, Sharma R, Bandari DK, et al. Prevalence of Polypharmacy, Hyperpolypharmacy and Potentially Inappropriate Medication Use in Older Adults in India: A Systematic Review and Meta-Analysis. Front Pharmacol. 2021;12:685518. PubMed PMID: 34093207.
Zamora-Sanchez JJ, Urpi-Fernandez AM, Sastre-Rus M, Lumillo-Gutierrez I, Gea-Caballero V, Jodar-Fernandez L, et al. The Tilburg frailty indicator: a psychometric systematic review. Ageing Res Rev. 2022; 76:101588. PubMed PMID: 35150901.
Radhakrishnan M, Nagaraja SB. Modified Kuppuswamy socioeconomic scale 2023: stratification and updates. Int J Community Med Public Health. 2023;10:4415-8.
Nari F, Park EC, Nam CM, Jang SI. Impact of frailty on mortality and healthcare costs and utilization among older adults in South Korea. Sci Rep. 2023;13:21203. PubMed PMID: 38040759.
Alqahtani B. Number of medications and polypharmacy are associated with frailty in older adults: results from the Midlife in the United States study. Front Public Health. 2023;11:1148671. PubMed PMID: 37304087.
Hajjar ER, Cafiero AC, Hanlon JT. Polypharmacy in elderly patients. Am J Geriatr Pharmacother. 2007;5: 345-51.
Delara M, Murray L, Jafari B, Bahji A, Goodarzi Z, Kirkham J, et al. Prevalence and factors associated with polypharmacy: a systematic review and meta-analysis. BMC Geriatr. 2022;22:601. PubMed PMID: 35854209.
Nguyen TX, Nguyen TN, Nguyen AT, Nguyen HT, Nguyen TT, Nguyen TN, et al. Polypharmacy at discharge in older hospitalised patients in Vietnam and its association with frailty. Australas J Ageing. 2020; 39:230-6.
Hosseini SR, Zabihi A, Amiri SR, Bijani A. Polypharmacy among the elderly. J Midlife Health. 2018;9:97-103.
Lai SW, Liao KF, Liao CC, Muo CH, Liu CS, Sung FC. Polypharmacy correlates with increased risk for hip fracture in the elderly: a population-based study. Medicine (Baltimore). 2010;89:295-9.
Gnjidic D, Hilmer SN, Blyth FM, Naganathan V, Waite L, Seibel MJ, et al. Polypharmacy cutoff and outcomes: five or more medicines were used to identify community-dwelling older men at risk of different adverse outcomes. J Clin Epidemiol. 2012;65:989-95.
Herr M, Sirven N, Grondin H, Pichetti S, Sermet C. Frailty, polypharmacy, and potentially inappropriate medications in old people: findings in a representative sample of the French population. Eur J Clin Pharmacol. 2017;73:1165-72.
Secora A, Alexander GC, Ballew SH, Coresh J, Grams ME. Kidney function, polypharmacy, and potentially inappropriate medication use in a community-based cohort of older adults. Drugs Aging. 2018;35:735-50.
Woo J, Yu R, Wong M, Yeung F, Wong M, Lum C. Frailty screening in the community using the FRAIL scale. J Am Med Dir Assoc. 2015;16:412-9.
Moore AA, Whiteman EJ, Ward KT. Risks of combined alcohol/medication use in older adults. Am J Geriatr Pharmacother. 2007;5:64-74.
Gangwar R, Kumar A, Zargar AA, Sharma A, Kumar R. The role of drug utilization evaluation in medical sciences. Glob Health J. 2023;7:3-8.
Zevin S, Benowitz NL. Drug interactions with tobacco smoking: an update. Clin Pharmacokinet. 1999;36:425-38.
Hamza SA, Saber HG, Hassan N. Relationship between sleep disturbance and polypharmacy among hospitalized elderly. Eur J Geriatr Gerontol. 2019;6:34-7.
Doumat G, Daher D, Itani M, Abdouni L, El Asmar K, Assaf G. The effect of polypharmacy on healthcare services utilization in older adults with comorbidities: a retrospective cohort study. BMC Prim Care. 2023; 24:120. PubMed PMID: 37237338
Nobili A, Garattini S, Mannucci PM. Multiple diseases and polypharmacy in the elderly: challenges for the internist of the third millennium. J Comorb. 2011;1:28-44.