Development of a YOLOv8-based deep learning framework for detection and classification of periapical radiolucencies in dental radiographs using the periapical index
Main Article Content
Abstract
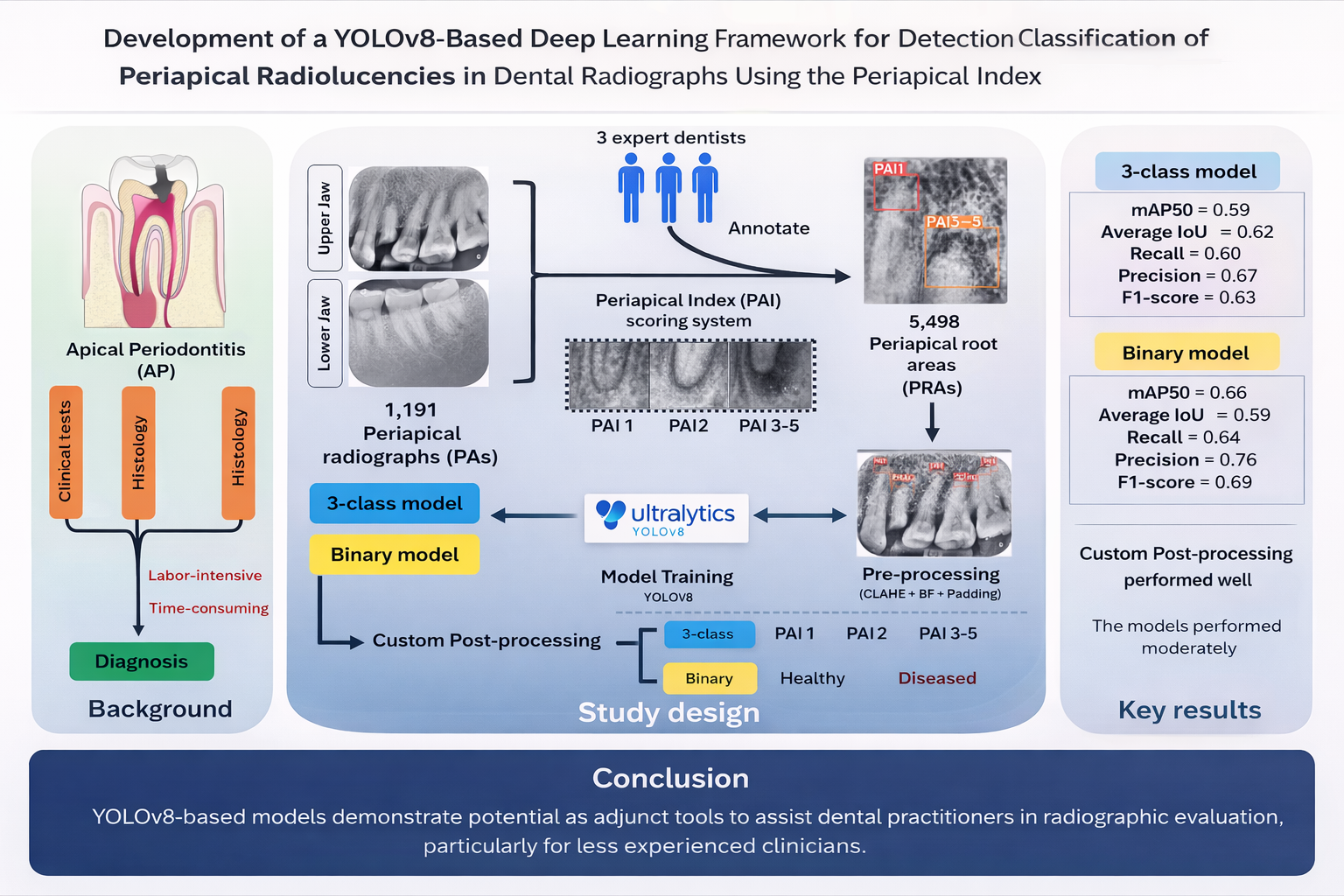
Background: Apical periodontitis (AP) is one of the most common oral diseases worldwide. Radiographs are widely used for diagnosing AP. However, their interpretation is subjective and time-consuming, contributing to increased clinical workload. Although deep learning has been introduced to assist diagnosis, most existing models are trained on limited sets of teeth, restricting their generalizability.
Objective: To investigate the potential of the YOLOv8 model for detecting and classifying periapical radiolucencies in periapical radiographs using the PAI criteria.
Materials and methods: A total of 1,191 periapical radiographs from both mandibular and maxillary jaws were collected and scored. Experts annotated 5,498 bounding boxes covering periapical root areas (PRAs). YOLOv8 models were developed to detect PRAs and classify PAI scores, which were grouped into three classes: PAI 1, PAI 2, and PAI 3-5. A custom post-processing method was implemented to improve inference by filtering overlapping detections. Filtered predictions from the test dataset were evaluated for both post-processing methods using precision, recall, F1-score, and mean average precision at an IoU threshold of 0.5 (mAP50). Confusion matrices were used to analyze misclassification patterns, while average IoU assessed overall detection performance.
Results: The best YOLOv8 model achieved a mean average precision at an intersection over union (IoU) threshold of 0.5 (mAP50) of 0.59 with a global average IoU of 0.62. A binary classification ablation model, grouping PAI 1-2 as “healthy” and PAI 3–5 as “diseased,” achieved an improved mAP50 of 0.66. The custom post-processing algorithm successfully eliminated all overlapping boxes and enhanced model performance.
Conclusions: Despite moderate performance, the YOLOv8-based models demonstrate potential as adjunct tools to assist dental practitioners in radiographic evaluation, particularly for less experienced clinicians. Further development is required to improve clinical applicability and robustness.
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Personal views expressed by the contributors in their articles are not necessarily those of the Journal of Associated Medical Sciences, Faculty of Associated Medical Sciences, Chiang Mai University.
References
Arias Z, Nizami MZI, Chen X, Xu B, Kuang C, Omori K, et al. Recent advances in apical periodontitis treatment: a narrative review. Bioengineering. 2023; 10(4):488. doi: 10.3390/bioengineering10040488.
Tibúrcio-Machado CS, Michelon C, Zanatta FB, Gomes MS, Marin JA, Bier CA. The global prevalence of apical periodontitis: a systematic review and meta-analysis. Int Endod J. 2021; 54(5): 712-35. doi: 10.1111/iej.13467.
Buonavoglia A, Zamparini F, Lanave G, Pellegrini F, Diakoudi G, Spinelli A, et al. Endodontic microbial communities in apical periodontitis. J Endod. 2023; 49(2): 178-89. doi: 10.1016/j.joen.2022.11.015
Loesche WJ. Microbiology of Dental Decay and Periodontal Disease. In: Baron S, Editor. Medical Microbiology. 4th Edition. Galveston, University of Texas Medical Branch at Galveston, Chapter 99.
Lo Giudice R, Nicita F, Puleio F, Alibrandi A, Cervino G, Lizio AS, et al. Accuracy of periapical radiography and CBCT in endodontic evaluation. Int J Dent. 2018; 2018:2514243. doi: 10.1155/2018/2514243.
Tanomaru-Filho M, Jorge EG, Duarte MA, Gonçalves M, Guerreiro-Tanomaru JM. Comparative radiographic and histological analyses of periapical lesion development. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009; 107(3): 442-7. doi: 10.1016/j.tripleo.2008.12.009.
Karamifar K, Tondari A, Saghiri MA. Endodontic periapical lesion: an overview on the etiology, diagnosis and current treatment modalities. Eur Endod J. 2020; 5(2): 54-67. doi: 10.14744/eej.2020.42714.
Ørstavik D, Kerekes K, Eriksen HM. The periapical index: a scoring system for radiographic assessment of apical periodontitis. Dent Traumatol. 1986; 2(1): 20-34. doi: 10.1111/j.1600-9657.1986.tb00119.x
Rajmohamed RF, Chapala S, Shazahan MA, Wali P, Botchu R. Evaluating the accuracy and efficiency of AI-generated radiology reports based on positive findings-a qualitative assessment of AI in radiology. Acad Radiol. 2025; 35(12): 7035-40. doi: 10.1016/j.acra.2025.09.012.
Kazimierczak N, Sultani N, Chwarścianek N, Krzykowski S, Janiszewska-Olszowska J, et al. Detection accuracy of an AI platform for dental treatment features on panoramic radiographs tooth- and patient-level analyses. Sci Rep, 2026; 16: 2436. doi: 10.1038/s41598-025-32226-0
Huang C, Wang J, Wang S, Zhang Y. A review of deep learning in dentistry. Neurocomputing. 2023; 554: 126629. doi: 10.1016/j.neucom.2023.126629.
Sohrabniya F, Hassanzadeh-Samani S, Ourang SA, Jafari B, Farzinnia G, Gorjinejad F, et al. Exploring a decade of deep learning in dentistry: a comprehensive mapping review. Clin Oral Invest. 2025; 29: 143. doi: 10.1007/s00784-025-06216-5.
Khan HA, Haider MA, Ansari HA, Ishaq H, Kiyani A, Sohail K, et al. Automated feature detection in dental periapical radiographs by using deep learning. Oral Surg Oral Med Oral Pathol Oral Radiol. 2021; 131(6): 711-20. doi: 10.1016/j.oooo.2020.08.024
Du M, Wu X, Ye Y, Fang S, Zhang H, Chen M. A combined approach for accurate and accelerated teeth detection on cone beam CT images. Diagnostics (Basel). 2022; 12(7): 1679. doi: 10.3390/diagnostics12071679.
Sadr S, Mohammad-Rahimi H, Motamedian SR, Zahedrozegar S, Motie P, Vinayahalingam S, et al. Deep learning for detection of periapical radiolucent lesions: a systematic review and meta-analysis of diagnostic test accuracy. J Endod. 2023; 49(3): 248-61.e3. doi: 10.1016/j.joen.2022.12.007.
Ver Berne J, Saadi SB, Politis C, Jacobs R. A deep learning approach for radiological detection and classification of radicular cysts and periapical granulomas. J Dent. 2023; 135: 104581. doi: 10.1016/j.jdent.2023.104581.
Moidu NP, Sharma S, Chawla A, Kumar V, Logani A. Deep learning for categorization of endodontic lesion based on radiographic periapical index scoring system. Clin Oral Investig. 2021; 26(1): 651-8. doi: 10.1007/s00784-021-04043-y.
Redmon J, Divvala S, Girshick R, Farhadi A. You only look once: unified, real-time object detection. Proceedings of the 2016 IEEE Conference on Computer Vision and Pattern Recognition (CVPR); 2016: 779-88. doi: 10.1109/CVPR.2016.91.
Sohan M, Sai Ram T, Rami Reddy ChV. A Review on YOLOv8 and its advancements. In: Jacob IJ, Piramuthu S, Falkowski-Gilski P, Editor. Data Intelligence and Cognitive Informatics. Singapore: Springer Nature; 2024: pp 529-45.
Singh K, Kumar R, Singh S. Advanced YOLOv8 architecture for multi-class brain tumor detection. J Assoc Med Sci [internet]. 2026 Feb. 25 [cited 2026 Mar. 20];59(2):250-8. available from: https://he01.tci-thaijo.org/index.php/bulletinAMS/article/view/281957.
Yaseen M. What is YOLOv8: an in-depth exploration of the internal features of the next-generation object detector. ArXiv Preprint posted online August 28, 2024. doi: 10.48550/arXiv.2408.15857.
Hirata N, Pudhieng P, Sena S, Torn-asa S, Panyarak W, Klanliang K, et al. Development of periapical index score classification system in periapical radiographs using deep learning. J Digit Imaging Inform Med. 2024; 38(5): 3125-33. doi: 10.1007/s10278-024-01360-y.
Bachani L, Singh M, Anshul, Lingappa A. Ideal radiographs: an insight. IP Int J Maxillofac Imaging. 2020; 6(3): 56-64. doi: 10.18231/j.ijmi.2020.017.
Choi JW, Han WJ, Kim EK. Image enhancement of digital periapical radiographs according to diagnostic tasks. Imaging Sci Dent. 2014; 44(1): 31-5. doi: 10.5624/isd.2014.44.1.31.
Ari T, Sağlam H, Öksüzoğlu H, Kazan O, Bayrakdar İŞ, Duman SB, et al. Automatic feature segmentation in dental periapical radiographs. Diagnostics. 2022; 12(12): 3081. doi: 10.3390/diagnostics12123081.
Chen IDS, Yang CM, Chen MJ, Chen MC, Weng RM, Yeh CH. Deep learning-based recognition of periodontitis and dental caries in dental X-ray images. Bioengineering (Basel). 2023; 10(8): 911. doi: 10.3390/bioengineering10080911.
Çelik B, Savaştaer EF, Kaya HI, Çelik ME. The role of deep learning for periapical lesion detection on panoramic radiographs. Dentomaxillofacial Radiol. 2023; 52(8): 20230118. doi: 10.1259/dmfr.20230118.s.
Taş İÇ. Application of panoramic dental x-Ray images denoising. Int J Innov Eng Appl. 2023; 7(1): 13-20. doi: 10.46460/ijiea.1134105.
Hana FM, Maulida ID. Analysis of contrast limited adaptive histogram equalization (CLAHE) parameters on finger knuckle print identification. J Phys Conf Ser. 2021; 1764(1): 012049. doi: 10.1088/1742-6596/1764/1/012049.
Ahmed S, Yoshiura N, Hassan S, Khan A. Towards better accuracy on imbalance image datasets using image augmentation and convolutional neural networks. Lecture Notes in Computer Science in International Conference on the Dynamics of Information Systems (LNCS-DIS 2024); 2025; 14661: 189-212. doi: 10.1007/978-3-031-81010-7_13.
Maia Filho EM, Calisto AM, De Jesus Tavarez RR, De Castri Rizzi C, Bezerra Segato RA, Bezerra da Silva LA. Correlation between the periapical index and lesion volume in cone-beam computed tomography images. Iran Endod J. 2018; 13(2): 155-8. doi: 10.22037/iej.v13i2.15040.
Mooijman P, Catal C, Tekinerdogan B, Lommen A, Blokland M. The effects of data balancing approaches: a case study. Appl Soft Comput. 2023; 132: 109853. doi: 10.1016/j.asoc.2022.109853.
Kawaguchi K, Kaelbling LP, Bengio Y. Generalization in deep learning. ArXiv Preprint posted online October 16, 2017. doi: 10.48550/arXiv.1710.05468.
Vakanski A, Xian M. Evaluation of complexity measures for deep learning generalization in medical image analysis. Proceedings of the 2021 IEEE 31st International Workshop on Machine Learning for Signal Processing (MLSP); 2021: 1-6. doi: 10.1109/mlsp52302.2021.9596501.