Combined neutrophil-to-lymphocyte, monocyte-to-lymphocyte, and platelet- to-lymphocyte ratios as inflammatory biomarkers in tuberculosis: A retrospective study from Lampang, Thailand
Main Article Content
Abstract
Background: Tuberculosis (TB) remains one of the major infectious diseases causing global morbidity and mortality. Systemic inflammation plays a central role in TB pathogenesis. Hematological indices derived from complete blood counts (CBC) including neutrophil-to-lymphocyte ratio (NLR), monocyte-to-lymphocyte ratio (MLR), and platelet-to-lymphocyte ratio (PLR) have been proposed as surrogate inflammatory biomarkers.
Objectives: To investigate the role of CBC-derived ratios (NLR, MLR, and PLR) as inflammatory biomarkers in TB patients compared with healthy controls, and to assess their association with clinical characteristics and laboratory findings.
Materials and methods: This retrospective study was conducted at Lampang Hospital, Thailand. Data from 213 TB patients and 170 healthy controls were collected from medical records and hematology reports. CBC-derived ratios were calculated and analyzed using Mann-Whitney U test, multivariate logistic regression adjusted for age, gender, and body mass index (BMI), and receiver operating characteristic (ROC) curve analysis.
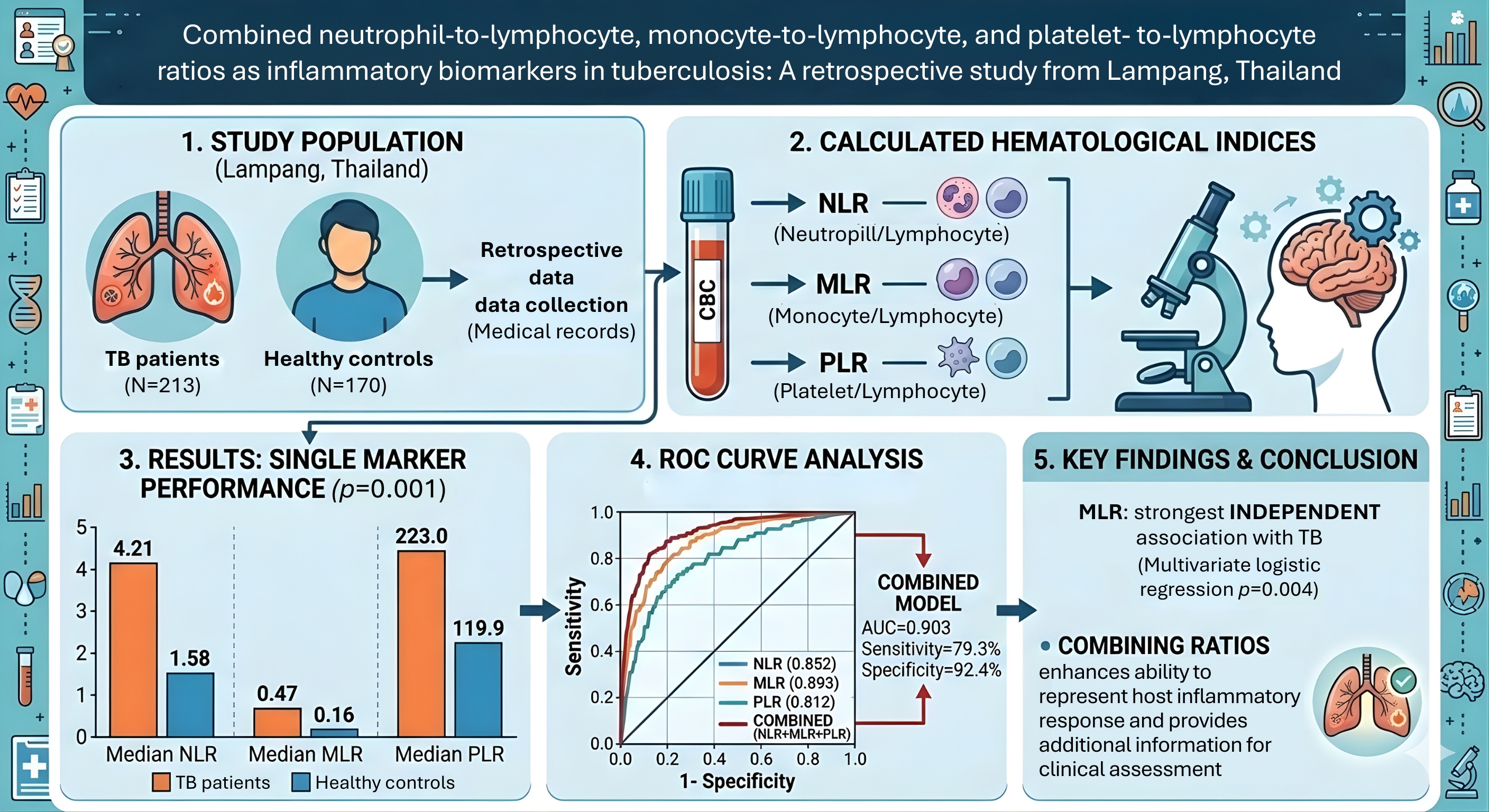
Results: Median NLR, MLR, and PLR values were significantly higher in TB patients compared with controls (NLR 4.21 vs 1.58; MLR 0.47 vs 0.16; PLR 223.0vs119.9; all p<0.001). In multivariate logistic regression analysis, only MLR (OR = 511.567; 95% CI: 7.384-35,439.660; p=0.004) remained independently associated with TB after adjustment, whereas NLR and PLR did not retain statistical significance. ROC analysis indicated good discrimination for NLR (AUC=0.852), MLR (AUC=0.893), and PLR (AUC=0.812). The combined model (NLR+MLR+PLR) achieved the highest accuracy (AUC=0.903; sensitivity=79.3%; specificity=92.4%).
Conclusion: Elevated NLR, MLR, and PLR values reflect systemic inflammation in TB patients. Among these markers, MLR showed the strongest independent association with TB. Although their specificity is limited, combining these ratios enhances their ability to represent the host inflammatory response and may provide additional information for clinical assessment and disease monitoring.
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Personal views expressed by the contributors in their articles are not necessarily those of the Journal of Associated Medical Sciences, Faculty of Associated Medical Sciences, Chiang Mai University.
References
Lv H, Wang L, Zhang X, Dang C, Liu F, Zhang X, et al. Further analysis of tuberculosis in eight highburden countries based on the Global Burden of Disease Study 2021 data. Infect Dis Poverty. 2024; 13(1): 70. doi: 10.1186/s40249-024-01247-8.
Yang H, Ruan X, Li W, Xiong J, Zheng Y. Global, regional, and national burden of tuberculosis and attributable risk factors for 204 countries and territories, 1990-2021: a systematic analysis for the Global Burden of Diseases 2021 study. BMC Public Health. 2024; 24(1): 3111. doi: 10.1186/s12889-024-20664-w.
Heyckendorf J, Georghiou SB, Frahm N, Heinrich N, Kontsevaya I, Reimann M, et al. Tuberculosis Treatment Monitoring and Outcome Measures: New Interest and New Strategies. Clin Microbiol Rev. 2022; 35(3): e0022721. doi: 10.1128/cmr.00227-21.
Yayan J, Franke KJ, Berger M, Windisch W, Rasche K. Early detection of tuberculosis: a systematic review. Pneumonia (Nathan). 2024; 16(1): 11. doi: 10.1186/s41479-024-00133-z.
Nyamagoud SB, Dsouza PD, Chitralu SPP, Solankure K, Swamy AHV. Evaluating hematological and inflammatory biomarkers in tuberculosis management. Monaldi Arch Chest Dis. 2025. doi: 10.4081/monaldi.2025.3433. Epub ahead of print.
Leo S, Narasimhan M, Rathinam S, Banerjee A. Biomarkers in diagnosing and therapeutic monitoring of tuberculosis: a review. Ann Med. 2024; 56(1): 2386030. doi: 10.1080/07853890.2024.2386030.
Adane T, Melku M, Ayalew G, Bewket G, Aynalem M, Getawa S. Accuracy of monocyte to lymphocyte ratio for tuberculosis diagnosis and its role in monitoring anti-tuberculosis treatment: Systematic review and meta-analysis. Medicine (Baltimore). 2022; 101(44): e31539. doi: 10.1097/MD.0000000000031539.
Tu HZ, Lai TJ, Chen YS, Lee HS, Chen JS. Hematological Parameters as Potential Markers for Distinguishing Pulmonary Tuberculosis from Genitourinary Tuberculosis. Pathogens. 2023; 12(1): 84. doi: 10.3390/pathogens12010084.
Obeagu EI. Inflammatory blood markers in breast cancer: a narrative review from early detection to therapy response. Ann Med Surg (Lond). 2025; 87(9): 5906-11. doi: 10.1097/MS9.0000000000003687.
Xue F, Li Z, Yan L, Yu Q, Zhang Y. The Correlation of Blood Immune Cells with the Pathogenesis of Schizophrenia: A Meta-Analysis. Iran J Public Health. 2025; 54(8): 1563-76. doi: 10.18502/ijph.v54i8.19566.
Omair M, Baig MS, Farooqui WA, Kousar S, Noori MY, Zeehan N, et al. Relationship of neutrophil lymphocyte ratio, monocyte lymphocyte ratio and neutrophil monocyte ratio with treatment response in pulmonary tuberculosis patients during intensive phase treatment. BMC Infect Dis. 2024; 24(1): 615. doi: 10.1186/s12879-024-09454-2.
Hua HB, Wang HJ. Monocyte-to-lymphocyte ratio is significantly associated with positive Quanti FERON-TB Gold-In-Tube and adult survival: an observational study. Sci Rep. 2022; 12(1): 20406. doi: 10.1038/s41598-022-24376-2.
Xiang ZB, Leng EL, Cao WF, Liu SM, Zhou YL, Luo CQ, et al. A systematic review and meta-analysis of the diagnostic accuracy of metagenomic next-generation sequencing for diagnosing tuberculous meningitis. Front Immunol. 2023; 14: 1223675. doi: 10.3389/fimmu.2023.1223675.
Shojaan H, Kalami N, Ghasempour Alamdari M, Emami Alorizy SM, Ghaedi A, Bazrgar A, et al. Diagnostic value of the neutrophil lymphocyte ratio in discrimination between tuberculosis and bacterial community acquired pneumonia: A meta-analysis. J Clin Tuberc Other Mycobact Dis. 2023; 33: 100395. doi: 10.1016/j.jctube.2023.100395.
Rahimirad S, Ghaffary MR, Rahimirad MH, Rashidi F. Association between admission neutrophil to lymphocyte ratio and outcomes in patients with acute exacerbation of chronic obstructive pulmonary disease. Tuberk Toraks. 2017; 65(1): 25-31.
Miyahara R, Piyaworawong S, Naranbhai V, Prachamat P, Kriengwatanapong P, Tsuchiya N, et al. Predicting the risk of pulmonary tuberculosis based on the neutrophil-to-lymphocyte ratio at TB screening in HIV-infected individuals. BMC Infect Dis. 2019; 19(1): 667. doi: 10.1186/s12879-019-4292-9.
Kaufmann SH. How can immunology contribute to the control of tuberculosis? Nat Rev Immunol. 2001;1(1):20-30. doi: 10.1038/35095558.
Scriba TJ, Coussens AK, Fletcher HA. Human Immunology of Tuberculosis. Microbiol Spectr. 2017; 5(1): TBTB2-0016-2016. doi: 10.1128/microbiolspec.tbtb2-0016-2016.
Hult C, Mattila JT, Gideon HP, Linderman JJ, Kirschner DE. Neutrophil Dynamics Affect Mycobacterium tuberculosis Granuloma Outcomes and Dissemination. Front Immunol. 2021; 12: 712457. doi: 10.3389/fimmu.2021.712457.
Weeratunga P, Moller DR, Ho LP. Immune mechanisms of granuloma formation in sarcoidosis and tuberculosis. J Clin Invest. 2024; 134(1): e175264. doi: 10.1172/JCI175264.
Chandra P, Grigsby SJ, Philips JA. Immune evasion and provocation by Mycobacterium tuberculosis. Nat Rev Microbiol. 2022; 20(12): 750-66. doi: 10.1038/s41579-022-00763-4.
Li F, Chen D, Zeng Q, Du Y. Possible Mechanisms of Lymphopenia in Severe Tuberculosis. Micro organisms. 2023; 11(11): 2640. doi: 10.3390/microorganisms11112640.
Xiao S, Ma X, Shi G, Zhou T, Pan J. Association between neutrophil-lymphocyte ratio and latent tuberculosis infection in the United States: a cross-sectional study from NHANES 2011-2012. BMC Infect Dis. 2025;25(1):1139. doi: 10.1186/s12879-025-11505-1.
Gulgun M. Assessment of Platelet-to-Lymphocyte Ratio Can Be Affected by Several Factors. Med Princ Pract. 2017; 26(3): 299-300. doi: 10.1159/000456664.
Kim MA, Park YE, Chong YP, Shim TS, Jo KW. Neutrophil-Lymphocyte Ratio and Monocyte-Lymphocyte Ratio According to the Radiologic Severity of Mycobacterium avium Complex Pulmonary Disease. J Korean Med Sci. 2022; 37(40): e292. doi: 10.3346/jkms.2022.37.e292.
M Y, Vamja R, Parmar PA, Makwana N, Sundar RNS. Haematological markers as predictive tools for tuberculosis in PLHIV: a retrospective cohort study in Gujarat, India. BMC Infect Dis. 2025; 25(1): 228. doi: 10.1186/s12879-025-10625-y.
Rees CA, Pineros DB, Amour M, Munseri P, Said J, Magohe A, et al. The potential of CBC-derived ratios (monocyte-to-lymphocyte, neutrophil-tolymphocyte, and platelet-to-lymphocyte) to predict or diagnose incident TB infection in Tanzanian adolescents. BMC Infect Dis. 2020; 20(1): 609. doi: 10.1186/s12879-020-05331-w.