Prevalence and characterization of β-thalassemia minor in a premarital screening at a hereditary blood diseases center in Babylon, Iraq
Main Article Content
Abstract
Background: β-thalassemia is a significant hereditary hematological disorder that is highly prevalent in Iraq. Premarital screening is a critical preventive strategy for identifying couples at risk of having children with thalassemia major. This study evaluated the effectiveness of a premarital screening program in Babylon, Iraq.
Objectives: To determine the prevalence of β -thalassemia minor among couples with abnormal red cell indices and characterize the associated hematological parameters.
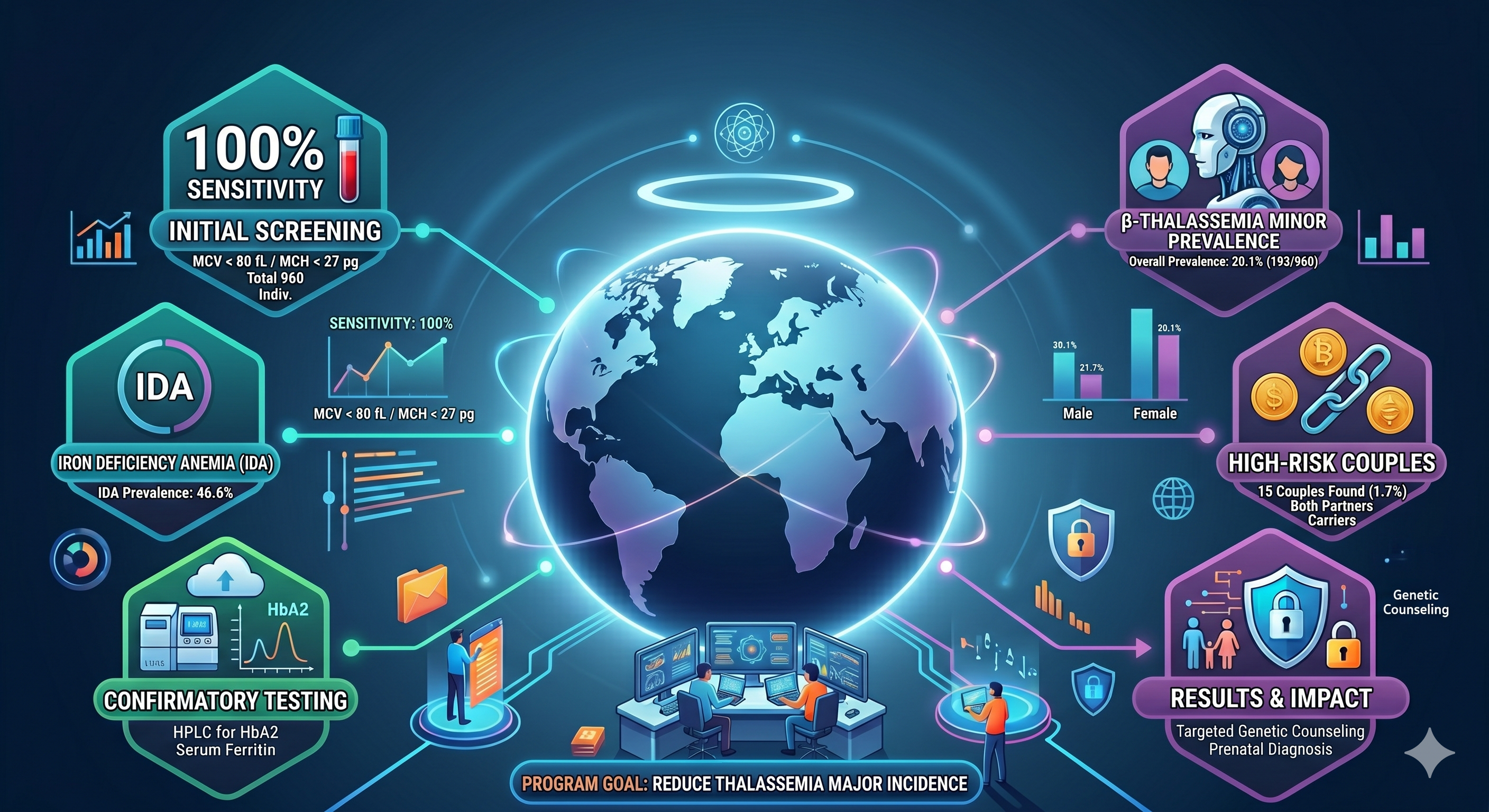
Materials and methods: A cross-sectional study was conducted from 2016 to 2019 on 960 individuals (480 couples) referred to the Hereditary Blood Diseases Center. Participants with a mean corpuscular volume (MCV) <80 fL and/or mean corpuscular hemoglobin (MCH) <27 pg underwent confirmatory testing via high-performance liquid chromatography (HPLC) for HbA2 quantification and serum ferritin analysis.
Results: The prevalence of β-thalassemia minor was 20.1% (193/960), with a significant sex disparity (males: 27.7%, females: 12.5%). Iron deficiency anemia (IDA) was identified in 46.6% of participants. The initial screening step using MCV/MCH cut-offs showed 100% sensitivity but 53.4% specificity, primarily because of IDA. Fifteen high-risk couples (1.7%) in which both partners were carriers were identified.
Conclusion: The two-stage premarital screening protocol demonstrated high sensitivity for detecting β-thalassemia carriers. The high prevalence of both the thalassemia trait and IDA in this young adult population underscores a substantial public health burden. The program successfully identified at-risk couples, enabling targeted genetic counseling and prenatal diagnosis to reduce the incidence of thalassemia major.
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Personal views expressed by the contributors in their articles are not necessarily those of the Journal of Associated Medical Sciences, Faculty of Associated Medical Sciences, Chiang Mai University.
References
Abd Al-Abbass HA, Obaid AF, Makki Al-Hindy H, Abdulrasol ZA, Jasim Shlash AM. Epidemiological characteristics and disease complications in thalassemia syndrome patients in Babylon, Iraq. J Babol Univ Med Sci. 2024; 26(1): 1-10. https://www.researchgate.net/profile/Hayder-Makki-5/publication/380178836.
Bellis G, Parant A. Beta-thalassemia in Mediterranean countries. Findings and outlook. Investig Geográficas. 2022; 77: 129-38. doi.org/10.14198/INGEO.19079.
Kattamis A, Forni GL, Aydinok Y, Viprakasit V. Changing patterns in the epidemiology of β-thalassemia. Eur J Haematol. 2020;105(6): 692-703. doi.org/10.1111/ejh.13512.
Abbas RA, Hassan RH, Taghlubee IM, Mohammed SI, Mohammed HH, Hasan HH, et al. Prevalence and molecular characterization of β-thalassemia in Kirkuk Province of Northern Iraq. Hemoglobin. 2024; 48(5): 308-3. doi.org/10.1080/03630269.2024.2418507.
Hassan MK, Abbas RA, Hassan RA, Taghlubee IM, Abd Al Majeed SS, Khaleel GA, et al. Prevalence and spectrum of β-thalassemia mutations in Baghdad, Iraq: Data from the premarital screening program. Hemoglobin. 2025;49(1): 31-7. doi: 10.1080/03630269.2024.2446360.
Al-Najafi WK. Premarital screening program for hemoglobinopathies in Karbala, Iraq. Karbala J Med. 2020;13(1)): 2293-300. https://journals.uokerbala.edu.iq/index.php/kj/article/view/737.
Hanoon BD, Khalf SA, Khalaf IA. Premarital screening program in Al-Nuaman Teaching Hospital. Iraqi J Med Sci. 2021; 19(2): 1-5. https://iraqijms.net/index.php/jms/article/view/788.
Al-Maaroof ZW, Al Sharifi LM. Associations between serum ferritin levels, Age-stratified hematological parameters, and hemoglobin A2 levels in Iraqi Beta thalassemia carriers. J Appl Hematol. 2025; 16(2): 111-7. doi: 10.4103/joah.joah_49_25.
Bordbar E, Taghipour M, Zucconi BE. Reliability of different RBC indices and formulas in discriminating between β-thalassemia minor and other microcytic hypochromic cases. Mediterr J Hematol Infect Dis. 2015; 7(1): e2015022. doi: 10.4084/MJHID.2015.022.
Kablan NM, El Hamshary MO, Nasr GM, Hamza MT, Salam TH, Hemeida AA. Hemoglobin A2 cut off values in Egyptian cohort as a marker of β-thalassemia carriers. J Biosci Appl Res. 2015; 1(4): 154-9. https://jbaar.journals.ekb.eg/article_106021.
Khera R, Singh T, Khuana N, Gupta N, Dubey AP. HPLC in characterization of hemoglobin profile in thalassemia syndromes and hemoglobinopathies: a clinicohematological correlation. Indian J Hematol Blood Transfus. 2015; 31(1): 110-5. doi: 10.1007/s12288-014-0409-x.
Al-Maaroof ZW, Al-Taee ZM. Assessment of anemia prevalence in urban populations: A communitybased study. J Appl Hematol. 2025; 16(1): 63-7. doi: 10.4103/joah.joah_128_24.
Al-Allawi NA, Al-Dousky AA. Frequency of haemoglobinopathies at premarital health screening in Dohuk, Iraq: implications for a regional prevention programme. East Mediterr Heal J. 2010; 16(4): 1-5. https://pubmed.ncbi.nlm.nih.gov/20795420/.
Al-Amodi AM, Ghanem NZ, Aldakeel SA, Ibrahim Al Asoom L, Rafique Ahmed N, Almandil NB, et al. Hemoglobin A2 (HbA2) has a measure of unreliability in diagnosing β-thalassemia trait (β-TT). Curr Med Res Opin. 2018; 34(5): 945-51. doi: 10.1080/03007995.2018.1435520.
Samanta A, Chaudhuri PK, Das U, Bhattacharyya N. A new approach based on erythrocyte indices to exclude normal populations from chromatography based thalassemia screening programs with very Hhgh fidelity. Iran J Blood Cancer. 2021; 13(4): 107-18. http://ijbc.ir/files/site1/user_files_6-10-667-1-c721e4c.pdf.
Organization WH. WHO guideline on use of ferritin concentrations to assess iron status in populations [Internet]. World Health Organization; 2020. https://iris.who.int/bitstream/handle/10665/331505/9789240000124.
Hashemizadeh H, Noori R. Premarital screening of beta thalassemia minor in North-East of Iran. Iran J Pediatr Hematol Oncol. 2013; 3(1): 210-5. PMID: 24575266
Khan AM, Al-Sulaiti AM, Younes S, Yassin M, Zayed H. The spectrum of beta-thalassemia mutations in the 22 Arab countries: a systematic review. Expert Rev Hematol. 2021; 14(1): 109-22. doi: 10.1080/17474086.2021.1860003
Mir SA, Alshehri BM, Alaidarous M, Banawas SS, Dukhyil AAA Bin, Alturki MK. Prevalence of hemoglobinopathies (β-thalassemia and sickle cell trait) in the adult population of Al Majma’ah, Saudi Arabia. Hemoglobin. 2020; 44(1): 47-50. doi.org/10.1080/03630269.2020.1729175.
Nezhad FH, Nezhad KH, Choghakabodi PM, Keikhaei B. Prevalence and genetic analysis of α- and β-thalassemia and sickle cell anemia in Southwest Iran. J Epidemiol Glob Health. 2018; 8(3): 189-95. doi.org/10.2991/j.jegh.2018.04.103
Sun A, Chang JYF, Jin YT, Chiang CP. Differential diagnosis between iron deficiency anemia and thalassemia trait-induced anemia. J Dent Sci. 2023; 18(4): 1963-4.doi: 10.1016/j.jds.2023.07.036.
Jameel T, Baig M, Ahmed I, Hussain MB, Alkhamaly MBD. Differentiation of beta thalassemia trait from iron deficiency anemia by hematological indices. Pakistan J Med Sci. 2017; 33(3): 665-9. doi: 10.12669/pjms.333.12098.
Mohammad SM, Algahtani MS, Alsharif AA, Alshehri RH, Ghali KN Bin, Al-Almaei HMF, et al. Awareness of iron deficiency anemia among the adult population in Riyadh, Saudi Arabia. Int J Med Dev Ctries. 2020; 4(12): 2259. Available from: https://ijmdc.com/fulltext/51-1603909600.
Heng GU, Wang YX, Du MX, Xu SS, Zhou BY, Li MZ. Effectiveness of using mean corpuscular volume and mean corpuscular hemoglobin for betathalassemia carrier screening in the Guangdong population of China. Biomed Environ Sci. 2021; 34(8): 667-71. doi: 10.3967/bes2021.094.
Sahiratmadja E, Maskoen AM, Reniarti L, Prihatni D. Erythrocyte indices MCV and/or MCH as first round screening followed by Hb-analysis for β-thalassemia carrier state. Indones Biomed J. 2022; 14(3): 282-8. doi.org/10.18585/inabj.v14i3.1960.
Sari DP, Wahidiyat PA, Setianingsih I, Timan IS, Gatot D, Kekalih A. Hematological parameters in individuals with beta thalassemia trait in South Sumatra, Indonesia. Anemia. 2022; 2022: 3572986. doi: 10.1155/2022/3572986.
Cao A, Kan YW. The prevention of thalassemia. Cold Spring Harb Perspect Med. 2013; 3(2): a011775. doi: 10.1101/cshperspect.a011775.
Owaidah T, Al-Numair N, Al-Suliman A, Zolaly M, Hasanato R, Al Zahrani F, et al. Iron deficiency and Iron deficiency anemia are common epidemiological conditions in Saudi Arabia: Report of the national epidemiological survey. Anemia. 2020; 2020: 6642568. doi: 10.1155/2020/6642568.
Saffi M, Howard N. Exploring the effectiveness of mandatory premarital screening and genetic counselling programmes for β-thalassaemia in the Middle East: A Scoping Review. Public Health Genom. 2015; 18(4): 193-203. doi: 10.1159/000430837.
Rouh AlDeen N, Osman AA, Alhabashi MJ, Al Khaldi R, Alawadi H, Alromh MK, et al. The prevalence of β-thalassemia and other hemoglobinopathies in Kuwaiti premarital screening program: An 11-year experience. J Pers Med. 2021; 11(10): 980. doi: https://www.mdpi.com/2075-4426/11/10/980.
Soteriades ES, Angastiniotis M, Economidou EC, Farmakis D, Avraam D, Eleftheriou A. The disease burden of β-thalassaemia revisited. Hematology. 2025; 30(1): 2551450. doi.org/10.1080/16078454.2025.2551450.
Pitsillidou O, Petrou P, Postma MJ. Can Cyprus afford luspatercept a budget impact analysis of the reimbursement of luspatercept for the management of thalassaemia in Cyprus. Pharmaco Economics-Open. 2024; 8(3): 471-80. doi: 10.1007/s41669-024-00482-x.
Rebeen Abdulsalam Mohammed Sediqm SASAA. Attitude and knowledge of participating couples towards the premarital hemoglobinopathy screening program in Duhok–Iraq. AMJ. 2024; 9(4): 84-93. doi.org/10.56056/amj.2024.302.
Hawi ZA, Pugsley K, Namipashaki A, Samarrai W, Hawi Z. A Review of Consanguinity in the Iraqi Population: A Call to Action to Prevent a Future Health Catastrophe. Ibn AL-Haitham J Pure Appl Sci . 2024; 37(2 SE-Biology): 64-70. doi.org/10.30526/37.2.3472.