The usefulness of endometrial receptivity biomarkers as predictors of IVF outcome
Main Article Content
Abstract
Background: Despite advances in assisted reproductive technology, predicting in vitro fertilization (IVF) success remains challenging.
Objectives: This study aimed to investigate the relationship between endometrial receptivity biomarkers and Ovarian Sensitivity Index (OSI) as predictors of IVF outcomes.
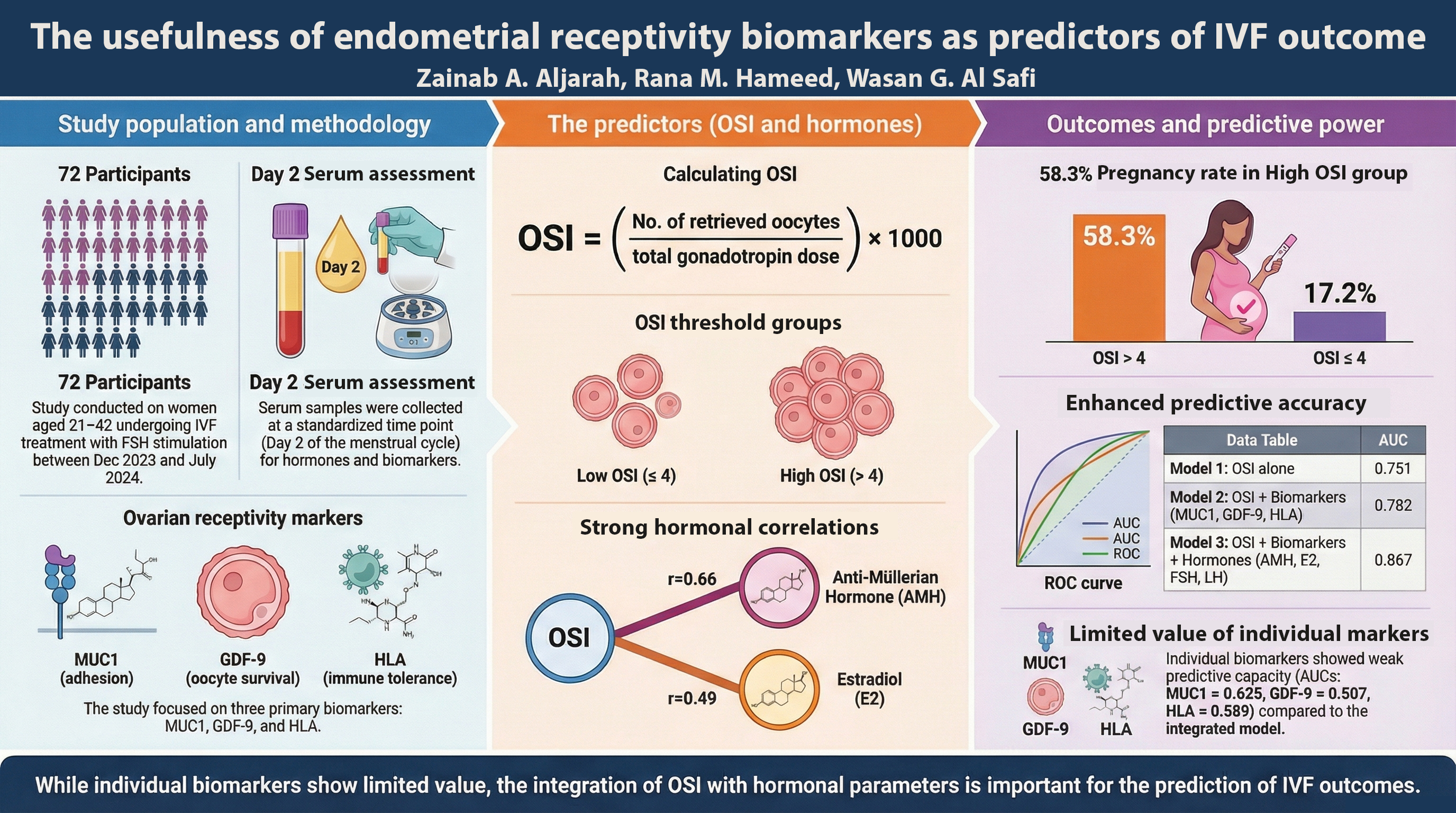
Materials and methods: A total of 72 women undergoing IVF treatment, between December 2023 and July 2024, participated in this study. Serum levels of MUC1, GDF-9, and HLA were measured, OSI was calculated, and pregnancy outcomes (β-hCG) were recorded. Participants were divided into two groups based on OSI (≤4 and >4), and biomarker levels were compared. Correlation analysis, ROC curves, and logistic regression models were used to assess predictive capabilities.
Results: OSI showed strong predictive value (AUC=0.751, 95% CI: 0.613-0.859, p<0.05) with a threshold of >8 (sensitivity=52.63%, specificity=94.12%). Endometrial biomarkers showed limited individual predictive capacity (AUCs: MUC1=0.625, GDF-9=0.507, HLA=0.589). OSI retained significant association with pregnancy outcomes across all regression models (OR=1.19-1.38, p<0.05). Combining hormonal parameters with OSI significantly improved model performance (AUC=0.867, R²=0.509). Significant correlations were observed between OSI and hormonal parameters, particularly AMH (r=0.66, p<0.05) and E2 (r=0.49, p<0.05).
Conclusion: While endometrial receptivity biomarkers showed limited individual predictive value, the incorporation of OSI with hormonal parameters provides better predictive value of IVF outcomes, suggesting the importance of a comprehensive assessment in assisted reproduction.
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Personal views expressed by the contributors in their articles are not necessarily those of the Journal of Associated Medical Sciences, Faculty of Associated Medical Sciences, Chiang Mai University.
References
Shingshetty L, Cameron NJ, Mclernon DJ, Bhattacharya S. Predictors of success after in vitro fertilization. Fertil Steril. 2024; 121: 742-51. doi: 10.1016/j.fertnstert.2024.03.003.
Yurci A. The impact of psychological factors on in vitro fertilization (IVF) outcomes: a comprehensive review. J Compr Surg. 2024; 2: 35-8. doi: 10.51271/JOCS-0031
Younglai E V., Holloway AC, Foster WG. Environmental and occupational factors affecting fertility and IVF success. Hum Reprod Update. 2005; 11: 43-57. doi: 10.1093/humupd/dmh055.
Hornstein MD. Lifestyle and IVF outcomes. Reprod Sci. 2016; 23: 1626-9. doi: 10.1177/1933719116667226.
Rienzi L, Cimadomo D, Vaiarelli A, Gennarelli G, Holte J, Livi C, et al. Measuring success in IVF is a complex multidisciplinary task: time for a consensus? Reprod Biomed Online. 2021; 43: 775-8. doi: 10.1016/j.rbmo.2021.08.012.
Sullivan-Pyke CS, Senapati S, Mainigi MA, Barnhart KT. In Vitro fertilization and adverse obstetric and perinatal outcomes. Semin Perinatol. 2017; 41: 345-53. doi: 10.1053/j.semperi.2017.07.001.
López-Luna A, Hernández-Melchor D, Ramírez-Martínez L, López-Bayghen E. The genetic and biochemical blueprint of endometrial receptivity: Past, present, and future factors involved in embryo implantation success. Modern medical genetics and genomics. IntechOpen; 2019.; ID:7904292.
Achache H, Revel A. Endometrial receptivity markers, the journey to successful embryo implantation. Hum Reprod Update. 2006; 12: 731-46. doi:10.1093/humupd/dml004.
Miravet-Valenciano JA, Rincon-Bertolin A, Vilella F, Simon C. Understanding and improving endometrial receptivity. Curr Opin Obstet Gynecol. 2015; 27:187-92. doi:10.1097/GCO.0000000000000173.
Brayman M, Thathiah A, Carson DD. MUC1: A multifunctional cell surface component of reproductive tissue epithelia. Reproductive Biology and Endocrinology. 2004; 2: No.4.
Hreinsson JG, Scott JE, Rasmussen C, Swahn ML, Hsueh AJW, Hovatta O. Growth differentiation factor-9 promotes the growth, development, and survival of human ovarian follicles in organ culture. J Clin Endocrinol Metab. 2002; 87: 316-21. doi:10.1210/jc.87.1.316.
Fountas S, Petinaki E, Bolaris S, Kargakou M, Dafopoulos S, Zikopoulos A, et al. The roles of GDF-9, BMP-15, BMP-4 and EMMPRIN in folliculogenesis and in vitro fertilization. J Clin Med. 2024; 13: 3775. doi.org/10.3390/cm13133775.
Chakravarty S, Kamal M. MUC1 and E-cadherin immunohistochemistry of endometrium cannot predict the outcome of in vitro fertilization: A case-control study. F1000Res. 2019; 8: 162.
Huang T, Chen F, Zhang Y, Chen S, Long F, Wei J, et al. Decreased GDF9 and BMP15 in follicle fluid and granulosa cells and outcomes of IVF-ET among young patients with low prognosis. J Assist Reprod Genet. 2023; 40: 567-76. doi: 10.1007/s10815-023-02723-0.
Li Y, Li R-Q, Ou S-B, Zhang N-F, Ren L, Wei L-N, et al. Increased GDF9 and BMP15 mRNA levels in cumulus granulosa cells correlate with oocyte maturation, fertilization, and embryo quality in humans. Reprod Biol Endocrinol. 2014; 12: 81. doi: 10.1186/1477-7827-12-81.
Peng L, Zhao W, Yin T, Xu C, Wang G, Du M. The unique expression pattern of human leukocyte antigen in trophoblasts potentially explains the key mechanism of maternal-fetal tolerance and successful pregnancy. J Reprod Immunol. 2023; 158: 103980. doi:10.1016/j.jri.2023.103980.
Zhuang B, Shang J, Yao Y. HLA-G: An important mediator of maternal-fetal immune-tolerance. Front Immunol. 2021 ; 12: 744324. doi.org/10.3389/fimmu.2021.744324
Revelli A, Gennarelli G, Biasoni V, Chiadò A, Carosso A, Evangelista F, et al. The ovarian sensitivity index (OSI) significantly correlates with ovarian reserve biomarkers, is more predictive of clinical pregnancy than the total number of oocytes and is consistent in consecutive IVF cycles. J Clin Med. 2020; 9: 1914. PMCID: PMC6486569. PMID: 31058052
Hu F, Wang X, Ren H, Lv Y, Li H, Liu S, et al. Ovarian sensitivity index can be used as a more sensitive indicator than follicular output rate to predict IVF/ICSI outcomes in patients of normal expected ovarian response stimulated with GnRH antagonist protocol. Hum Fertil. 2023; 26: 1264-70. doi:10.1080/14647273.2023.2164869.
World Health Organization. WHO laboratory manual for the examination and processing of human semen. Geneva, Switzerland: WHO Press; 2010.
Biasoni V, Patriarca A, Dalmasso P, Bertagna A, Manieri C, Benedetto C, et al. Ovarian sensitivity index is strongly related to circulating AMH and may be used to predict ovarian response to exogenous gonadotropins in IVF. Reprod Biol Endocrinol. 2011; 9: 112. doi: 10.1186/1477-7827-9-112.
Weghofer A, Barad DH, Darmon SK, Kushnir VA, Albertini DF, Gleicher N. The ovarian sensitivity index is predictive of live birth chances after IVF in infertile patients. Hum Reprod Open. 2020; 2020(4): hoaa049. doi: 10.1093/hropen/hoaa049
Li HWR, Lee VCY, Ho PC, Ng EHY. Ovarian sensitivity index is a better measure of ovarian responsiveness to gonadotrophin stimulation than the number of oocytes during in-vitro fertilization treatment. J Assist Reprod Genet. 2014; 31: 199-203. doi: 10.1007/s10815-013-0144-5.
Bastu E, Mutlu MF, Yasa C, Dural O, Nehir Aytan A, Celik C, et al. Role of Mucin 1 and Glycodelin A in recurrent implantation failure. Fertil Steril. 2015; 103: 1059-1064.e2. doi: 10.1016/j.fertnstert. 2015.01.025.
Wu F, Chen X, Liu Y, Liang B, Xu H, Li TC, et al. Decreased MUC1 in endometrium is an independent receptivity marker in recurrent implantation failure during implantation window. Reproductive Biology and Endocrinology. 2018; 16: 60. doi: 10.1186/s12958-018-0379-1.
Hviid TVF, Hylenius S, Lindhard A, Christiansen OB. Association between human leukocyte antigen‐G genotype and success of in vitro fertilization and pregnancy outcome. Tissue Antigens. 2004; 64: 66-9. doi: 10.1111/ j.1399-0039.2004.00239.x.