Obesity risk and body composition among Bangkok adolescents with autism spectrum disorder: Stratification by sensory and cognitive severity using data mining
Main Article Content
Abstract
Background: Obesity is prevalent among children with autism spectrum disorder (ASD) and may worsen core symptoms. The unique challenges faced by this population may heighten their vulnerability to both general and ASD-specific obesity risk factors.
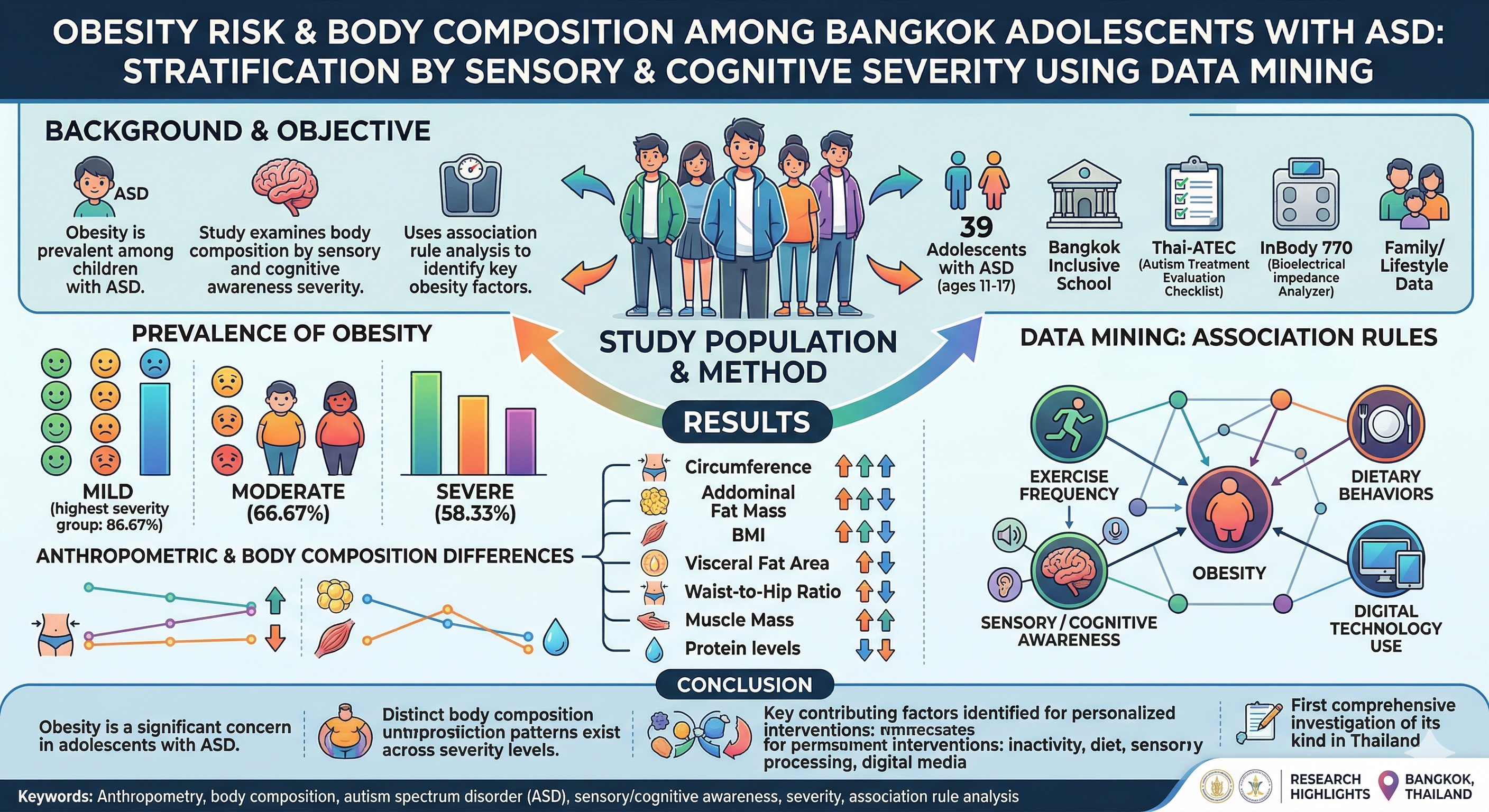
Objectives: This study examines body composition in adolescents with ASD, stratified by sensory and cognitive awareness severity and uses association rule analysis to identify key obesity-related factors for targeted intervention.
Materials and methods: This cross-sectional study was conducted at an inclusive school in Bangkok, Thailand, with 39 children aged 11-17 years diagnosed with ASD and their parents. ASD severity was assessed using the Thai Autism Treatment Evaluation Checklist (Thai-ATEC), and participants were categorized by sensory and cognitive awareness scores. Anthropometric data and body composition were measured using a bioelectrical impedance analyzer (InBody 770). BMI percentiles and body composition parameters such as body fat mass, skeletal muscle mass, and visceral fat area were recorded. Family and lifestyle data were also collected. Association rule analysis using a data mining technique was applied to explore variables linked to obesity.
Results: Different sensory/cognitive awareness severity levels (ATEC) had varying prevalences of obesity; the Mild group had the highest prevalence (86.67%), followed by the Moderate (66.67%) and Severe (58.33%) groups. The mild group consistently exhibited greater values for circumference, abdominal fat mass, body mass index, visceral fat area, waist-to-hip ratio, intracellular and extracellular water, skeletal muscle mass, and protein levels, indicating significant differences in anthropometric and body composition variables. Association rule analysis identified factors frequently linked to obesity, including exercise frequency, dietary behaviors, sensory/cognitive awareness severity, and digital technology use.
Conclusion: This study highlights obesity as a significant concern among adolescents with ASD with distinct body composition patterns across sensory/cognitive awareness severity levels. As the first comprehensive investigation of its kind in Thailand, it identifies key contributing factors-such as physical inactivity, dietary habits, sensory processing differences, and digital media use-underscoring the need for personalized, lifestyle-based interventions in this population.
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Personal views expressed by the contributors in their articles are not necessarily those of the Journal of Associated Medical Sciences, Faculty of Associated Medical Sciences, Chiang Mai University.
References
Zeidan J, Fombonne E, Scorah J, Ibrahim A, Durkin MS, Saxena S, et al. Global prevalence of autism: A systematic review update. Autism Res. 2022; 15(5): 778-90. doi:10.1002/aur.2696.
Okoye C, Obialo-Ibeawuchi CM, Obajeun OA, Sarwar S, Tawfik C, Waleed MS, et al. Early diagnosis of autism spectrum disorder: A review and analysis of the risks and benefits. Cureus. 2023; 15(8). doi:10.7759/cureus.43226.
Mano-Sousa BJ, Pedrosa AM, Alves BC, Galduróz JCF, Belo VS, Chaves VE, et al. Effects of risperidone in autistic children and young adults: a systematic review and meta-analysis. Curr Neuropharmacol. 2021; 19(4): 538-52. doi:10.2174/1570159X18666200529151741.
Scahill L, Jeon S, Boorin SJ, McDougle CJ, Aman MG, Dziura J, et al. Weight gain and metabolic consequences of risperidone in young children with autism spectrum disorder. J Am Acad Child Adolesc Psychiatry. 2016; 55(5): 415-23. doi:10.1016/j.jaac.2016.02.016.
Durkin MS, Maenner MJ, Newschaffer CJ, Lee L, Cunniff CM, Daniels JL, et al. Advanced parental age and the risk of autism spectrum disorder. Am J Epidemiol. 2008; 168(11): 1268-76. doi:10.1093/ aje/kwn250.
American Psychiatric Association. Diagnostic and statistical manual of mental disorders: DSM-5. 5th Ed. 2013. doi:10.1176/appi.books.9780890425596.
Ho HH, Eaves LC, Peabody D. Nutrient intake and obesity in children with autism. Focus Autism Dev Dis. 1997; 12(3): 187-92. doi:10.1177/108835769701200308.
Egan AM, Dreyer ML, Odar CC, Beckwith M, Garrison CB. Obesity in young children with autism spectrum disorders: prevalence and associated factors. Child Obes. 2013; 9(2): 125-31. doi:10.1089/chi.2012.0028.
Curtin C, Jojic M, Bandini LG. Obesity in children with autism spectrum disorder. Harv Rev Psychiatry. 2014; 22(2): 93-103. doi:10.1097/HRP.0000000000000031.
Bandini LG, Anderson SE, Curtin C, Cermak S, Evans EW, Scampini R, et al. Food selectivity in children with autism spectrum disorders and typically developing children. J Pediatr. 2010; 157(2): 259-64. doi:10.1016/j.jpeds.2010.02.013.
Ferguson BJ, Marler S, Altstein LL, et al. Psychophysiological associations with gastrointestinal symptomatology in autism spectrum disorder. Autism Res. 2017; 10(2): 276-88. doi:10.1002/aur.1646.
Dhaliwal KK, Orsso CE, Richard C, Haqq AM, Zwaigenbaum L. Risk factors for unhealthy weight gain and obesity among children with autism spectrum disorder. Int J Mol Sci. 2019; 20(13): 3285. doi:10.3390/ijms20133285.
Curtin C, Anderson SE, Must A, Bandini L. The prevalence of obesity in children with autism: a secondary data analysis using nationally representative data from the national survey of children's health. BMC Pediatr. 2010; 10: 1-5. doi:10.1186/1471-2431-10-11.
de Vinck-Baroody O, Shui A, Macklin EA, Hyman SL, Leventhal JM, Weitzman C. Overweight and obesity in a sample of children with autism spectrum disorder. Acad Pediatr. 2015; 15(4): 396-404. doi: 10.1016/j.acap.2015.03.008.
Zulkifli MN, Kadar M, Hamzaid NH. Weight status and associated risk factors of mealtime Behaviours among children with autism spectrum disorder. children. 2022; 9(7): 927. doi:10.3390/children9070927.
Kittana M, Ahmadani A, Williams KE, Attlee A. Nutritional atatus and feeding behavior of children with autism spectrum disorder in the Middle East and North Africa region. A Systematic review Nutrients. 2023; 15(3): 711. doi:10.3390/nu15030711.
Granich J, Lin A, Hunt A, Wray J, Dass A, Whitehouse AJ. Obesity and associated factors in youth with an autism spectrum disorder. Autism. 2016; 20(8): 916-26. doi:10.1177/1362361315616345.
Kantawala B, Abu-Bakr A, Kasini B, Ndayambaje M, Soh SI, Nazir A, et al. Exploring the landscape of autism in Africa: challenges in diagnosis, support, and resources–a short communication. Ann Med Surg. 2023; 85(11): 5838-41. doi:10.1097/MS9.0000000000001376.
Doreswamy S, Bashir A, Guarecuco JE, Lahori S, Baig A, Narra LR, et al. Effects of diet, nutrition, and exercise in children with autism and autism spectrum disorder: A literature review. Cureus. 2020; 12(12). doi: 10.7759/cureus.12222.
Tomchek SD, Dunn W. Sensory processing in children with and without autism: a comparative study using the short sensory profile. Am J Occup Ther. 2007; 61(2): 190-200. doi:10.5014/ajot.61.2.190.
Androutsos O, Zampelas A. Body composition in children: What does it tell us so far? Children. 2022; 9(8): 1199. doi:10.3390/children9081199.
Asia-Pacific Development Center on Disability. Autism at a Glance in ASEAN Under the Autism Mapping Project in the ASEAN Region: Part II Country Profiles. Bangkok: Thailand: Asia-Pacific Development Center on Disability Foundation; 2020 [Available from: https://efaidnbmnnnibpcajpcgl clefindmkaj/https://www.apcdfoundation.org/sites/ default/files/2020-09/AW_Autism%20at%20a%20Glance_Part%20II.pdf.
Khongpiboonkit R, Chaiyakit N, Wannapaschaiyong P, Sittanomai N. Prevalence and Factors Associated with Overweight and Obesity in Thai Children and Adolescents with Autism Spectrum Disorder: A Retrospective Longitudinal Study. J Autism Dev Disord. 2025. doi: 10.1007/s10803-025-06974-x
Agrawal R, Imieliński T, Swami A. Mining association rules between sets of items in large databases. In Proceedings of the 1993 ACM SIGMOD international conference on Management of data: 207-216.
Tan PN, Steinbach M, Kumar V. Introduction to data mining. Pearson Education India; 2016.
American Psychiatric Association. Diagnostic and statistical manual of mental disorders: DSM-IV-TR®.2000.
Sunakarach K, Kessomboon P. Validity and reliability of the Thai version of the Autism Treatment Evaluation Checklist: A two-phase diagnostic accuracy study. F1000Research. 2018; 7: 538.
WHO Expert Committee. Physical status : the use of and interpretation of anthropometry , report of a WHO expert committee. World Health Organ Tech Rep Ser. 1995: 312-44.
Tomczak M, Tomczak E. The need to report effect size estimates revisited. Trends Sport Sci. 2014; 21(1): 19-25.
Sasayama D, Kuge R, Toibana Y, Honda H. Trends in autism spectrum disorder diagnoses in Japan, 2009 to 2019. JAMA Network Open. 2021; 4(5): e219234-. doi:10.1001/jamanetworkopen.2021.9234.
Broder-Fingert S, Brazauskas K, Lindgren K, Iannuzzi D, Van Cleave J. Prevalence of overweight and obesity in a large clinical sample of children with autism. Acad Pediatr. 2014; 14(4): 408-14. doi:10.1016/j.acap.2014.04.004.
Zuckerman KE, Hill AP, Guion K, Voltolina L, Fombonne E. Overweight and obesity: prevalence and correlates in a large clinical sample of children with autism spectrum disorder. J Autism Dev Disord. 2014; 44: 1708-19. doi:10.1007/s10803-014-2050-9.
Cermak SA, Curtin C, Bandini LG. Food selectivity and sensory sensitivity in children with autism spectrum disorders. J Am Diet Assoc. 2010; 110(2): 238-46. doi: 10.1016/j.jada.2009.10.032.
Sharp WG, Berry RC, McCracken C, Nuhu NN, Marvel E, Saulnier CA, et al. Feeding problems and nutrient intake in children with autism spectrum disorders: a meta-analysis and comprehensive review of the literature. J Autism Dev Disord. 2013; 43: 2159-73. doi:10.1007/s10803-013-1771-5.
Lockner DW, Crowe TK, Skipper BJ. Dietary intake and parents' perception of mealtime behaviors in preschool-age children with autism spectrum disorder and in typically developing children. J Am Diet Assoc. 2008; 108(8): 1360-3. doi:10.1016/j.jada.2008.05.003.
Evans EW, Must A, Anderson SE, Curtin C, Scampini R, Maslin M, et al. Dietary patterns and body mass index in children with autism and typically developing children. Res Autism Spectr Disord 2012; 6(1): 399-405. doi:10.1016/j.rasd.2011.06.014.
Hyman SL, Stewart PA, Schmidt B, Cain U, Lemcke N, Foley JT, et al. Nutrient intake from food in children with autism. Pediatrics. 2012; 130(Supplement_2): S145-S53. doi:10.1542/peds.2012-0900L.
Corvey K, Menear KS, Preskitt J, Goldfarb S, Menachemi N. Obesity, physical activity and sedentary behaviors in children with an autism spectrum disorder. Matern Child Health J 2016; 20: 466-76. doi:10.1007/s10995-015-1844-5.
McCoy SM, Jakicic JM, Gibbs BB. Comparison of obesity, physical activity, and sedentary behaviors between adolescents with autism spectrum disorders and without. J Autism Dev Disord 2016; 46: 2317-26. doi:10.1007/s10803-016-2762-0.
Bandini LG, Curtin C, Phillips S, Anderson SE, Maslin M, Must A. Changes in food selectivity in children with autism spectrum disorder. J Autism Dev Disord 2017; 47: 439-46. doi: 10.1007/s10803-016-2963-6.
Matheson BE, Douglas JM. Overweight and obesity in children with autism spectrum disorder (ASD): A critical review investigating the etiology, development, and maintenance of this relationship. Rev J Autism Dev Disord 2017; 4(2): 142-56. doi:10.1007/s40489-017-0103-7.
O'Flaherty M, Hill J, Bourke M, Fortnum K, Thomas G, Gomersall SR, et al. Unpacking the relationship between autism, sport participation, and adolescent health: A causal mediation analysis. Disabil Health J. 2025; 3: 101832. doi: 10.1016/j.dhjo.2025.101832.
Arkesteyn A, Van Damme T, Thoen A, Cornelissen correlates in children and adolescents with autism spectrum disorder: a systematic review. Disabil Rehabil. 2022; 44(22): 6539-50. doi:10.1080/09638288.2021.1970251.