Fall incidence and associated factors in spinal cord injury patients who walk with or without an ambulatory assistive device
Main Article Content
Abstract
Background: The majority of ambulatory individuals with spinal cord injury (SCI) require an ambulatory assistive device (AAD). However, the association between falls and gait aid use is still inconsistent. Subgroup analysis may provide the opportunity to differentiate these factors more clearly.
Objectives: This study aimed to explore fall incidence and associated factors in SCI patients who walk with or without an AAD.
Materials and methods: Ninety-seven participants were interviewed for their baseline demographic data, physical activity, history of falling and fear of falling. They were divided into 2 groups, AAD and non AAD group. They were assessed with three functional tests, including the Timed Up and Go Test, Five Time Sit to Stand Test and 10 Meter Walk Test. Then fall data was followed for six months.
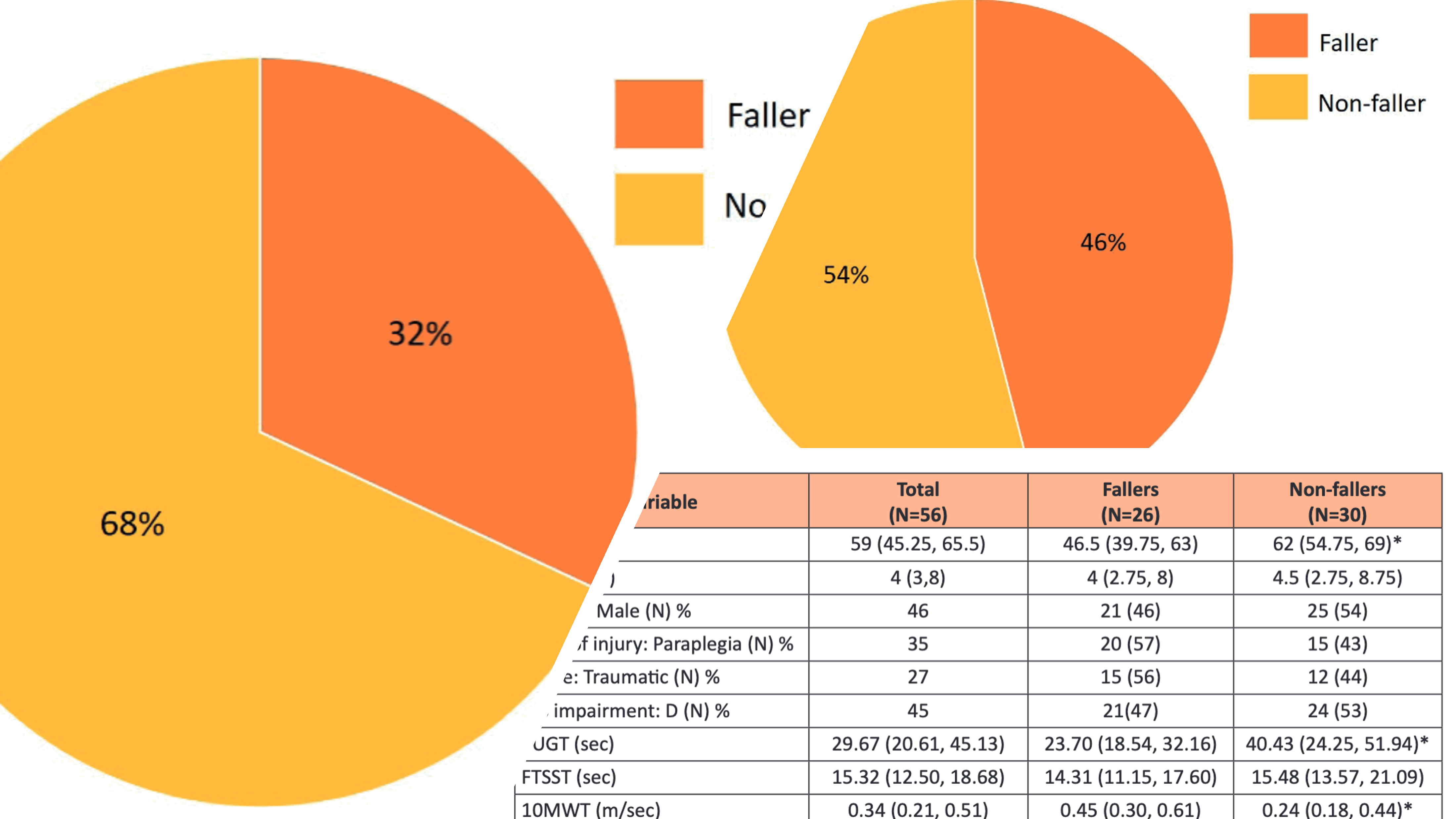
Results: More than one-third of all participants experienced at least one fall (40%). The results also showed that the proportion of falls in the AAD group was slightly greater than that of the non-AAD group (AAD=46% and non-AAD=32%). In the AAD group, a multiple variable analysis indicated a significantly higher fall rate among those who were younger than 50 years, used a cane or crutches and had moderate to high physical activity. For the non-AAD group, it was found that poor balance and a history of falls were strong factors associated with more falls.
Conclusion: Falls were a serious issue for the participants who walk with or without an ADD. However, the factors affecting falls in these two groups were different. Thus, therapists should consider the factors associated with falls for each group of SCI patients separately to provide proper rehabilitation that prevents falls and subsequent injury.
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Personal views expressed by the contributors in their articles are not necessarily those of the Journal of Associated Medical Sciences, Faculty of Associated Medical Sciences, Chiang Mai University.
References
Burns SP, Golding DG, Rolle WA, Graziani V, Ditunno JF. Recovery of ambulation in motor-incomplete tetraplegia. Arch Phys Med Rehabil. 1997; 78: 1169-72. doi: 10.1016/s0003-9993(97)90326-9.
Saensook W, Phonthee S, Srisim K, Mato L, Wattanapan P, Amatachaya S. Ambulatory assistive devices and walking performance in patients with incomplete spinal cord injury. Spinal Cord. 2014; 52: 216-9. doi: 10.1038/sc.2013.120.
Bateni H, Maki BE. Assistive devices for balance and mobility: benefits, demands, and adverse consequences. Arch Phys Med Rehabil. 2005; 86: 134-45. doi: 10.1016/j.apmr.2004.04.023.
Tagawa Y, Shiba N, Matsuo S, Yamashita T. Analysis of human abnormal walking using a multi-body model: joint models for abnormal walking and walking aids to reduce compensatory action. J Biomech. 2000; 33: 1405-14. doi: 10.1016/s0021-9290(00)00111-1.
Cruz AO, Santana SMM, Costa CM, Gomes da Costa LV, Ferraz DD. Prevalence of falls in frail elderly users of ambulatory assistive devices: A comparative study. Disabil Rehabil Assist Technol. 2020; 15: 510-14. doi: 10.1080/17483107.2019.1587016.
Phonthee S, Saengsuwan J, Siritaratiwat W, Amatachaya S. Incidence and factors associated with falls in independent ambulatory individuals with spinal cord injury: a 6-month prospective study. Phys Ther. 2013; 93: 1061-72. doi: 10.2522/ptj.20120467.
Phonthee S, Saengsuwan J, Amatachaya S. Falls in independent ambulatory patients with spinal cord injury: incidence, associated factors and levels of ability. Spinal Cord. 2013; 51(5): 365-8. doi: 10.1038/sc.2012.147.
Bu F, Abell J, Zaninotto P, Fancourt D. A longitudinal analysis of loneliness, social isolation and falls amongst older people in England. Sci Rep. 2020; 10: 20064. doi: 10.1038/s41598-020-77104-z.
Musselman KE, Arora T, Chan K, Alavinia M, Bone M, Unger J, et al. Evaluating intrinsic fall risk factors after incomplete spinal cord injury: distinguishing fallers from nonfallers. Arch Rehabil Res Clin Transl. 2021; 3: 100096. doi: 10.1016/j.arrct.2020.100096.
Saunders LL, Krause JS, DiPiro ND, Kraft S, Brotherton S. Ambulation and complications related to assistive devices after spinal cord injury. J Spinal Cord Med. 2013; 36: 652-9. doi: 10.1179/2045772312Y.0000000082
Brotherton SS, Krause JS, Nietert PJ. A pilot study of factors associated with falls in individuals with incomplete spinal cord injury. J Spinal Cord Med. 2007; 30: 243-50. doi: 10.1080/10790268.2007.11753932.
Jørgensen V, Butler Forslund E, Opheim A, Franzén E, Wahman K, Hultling C, et al. Falls and fear of falling predict future falls and related injuries in ambulatory individuals with spinal cord injury: a longitudinal observational study. J Physiother. 2017; 63: 108-13. doi: 10.1016/j.jphys.2016.11.010.
Brotherton SS, Krause JS, Nietert PJ. Falls in individuals with incomplete spinal cord injury. Spinal Cord. 2007; 45: 37-40. doi: 10.1038/sj.sc.3101909.
Verschuren O, Mead G, Visser-Meily A. Sedentary behaviour and stroke: foundational knowledge is crucial. Transl Stroke Res. 2015; 6(1): 9-12. doi:10.1007/s12975-014-0370-x.
Shumway-Cook A, Brauer S, Woollacott M. Predicting the probability for falls in community-dwelling older adults using the Timed Up & Go Test. Phys Ther. 2000; 80(9): 896-903. doi: 10.1093/ptj/77.8.812.
Graham JE, Ostir GV, Fisher SR, Ottenbacher KJ. Assessing walking speed in clinical research: a systematic review. J Eval Clin Pract. 2008; 14(4): 552-62. doi 10.1111/j.1365-2753.2007.00917.x.
Lord SR, Murray SM, Chapman K, Munro B, Tiedemann A. Sit-to-stand performance depends on sensation, speed, balance, and psychological status in addition to strength in older people. J Gerontol A Biol Sci Med Sci. 2002; 57(8): 539-43. doi 10.1093/gerona/57.8.m539.
Amatachaya S, Wannapakhe J, Arrayawichanon P, Siritarathiwat W, Wattanapun P. Functional abilities, incidences of complications and falls of patients with spinal cord injury 6 months after discharge. Spinal Cord. 2011; 49: 520-4. doi: 10.1038/sc.2010.163.
Roman de Mettelinge T, Cambier D. Understanding the relationship between walking aids and falls in older adults: A prospective cohort study. J Geriatr Phys Ther. 2015; 38: 127-32. doi: 10.1519/JPT.0000000000000031.
Matsuda P, Verrall A, Finlayson M, Molton I, Jensen M. Falls among adults aging with disability. Arch Phys Med Rehabil. 2015; 96: 464-71. doi: 10.1016/j.apmr.2014.09.034.
Jørgensen V, Butler Forslund E, Franzén E, Opheim A, Seiger Å, Ståhle A, et al. Factors associated with recurrent falls in individuals with traumatic spinal cord injury: a multicenter study. Arch Phys Med Rehabil. 2016; 97: 1908-16. doi: 10.1016/j.apmr.2016.04.024.
Liu-Ambrose T, Khan KM, Eng JJ, Janssen PA, Lord SR, Mckay HA. Resistance and agility training reduce fall risk in women aged 75 to 85 with low bone mass: a 6-month randomized, controlled trial. J Am Geriatr Soc. 2004; 52: 657-65. doi: 10.1111/j.1532-5415.2004.52200.x.
Lord S, Tiedemann A, Chapman K, Ther G, Munro B, Murray S, et al. The effect of an individualized fall prevention program on fall risk and falls in older people: a randomized, controlled trial. J Am Geriatr Soc. 2005; 53: 1296-304. doi: 10.7759/cureus.23713.
Faruqui SR, Jaeblon T. Ambulatory assistive devices in orthopaedics: uses and modifications. J Am Acad Orthop Surg. 2010; 18: 10. doi: 10.5435/00124635- 201001000-00006.
Brotherton SS, Saunders LL, Krause JS, Morrisette DC. Association between reliance on devices and people for walking and ability to walk community distances among persons with spinal cord injury. J Spinal Cord Med. 2012; 35: 156-61. doi: 10.1179/2045772312Y.0000000012.
Wright DL, Kemp TL. The dual-task methodology and assessing the attentional demands of ambulation with walking devices. Phys Ther. 1992; 72: 306-12. doi: 10.1093/ptj/72.4.306.
Neumann, DA., Hase, AD. An electromyographic analysis of the hip abductors during load carriage: implications for hip joint protection. JOSPT. 1994; 19(5): 296-304. doi: 10.2519/jospt.1994.19.5.296.
Thys, H., Willems, PA., Saels, P. Energy cost, mechanical work and muscular efficiency in swing-through gait with elbow crutches. J Biomechanics. 1996; 29(11): 1473-82. doi:10.1016/0021-9290(96)84543-x.
Moran J, Murphy A, Murphy D, Austin A, Moran D, Cronin C, et al. The energy expenditure of non-weight bearing crutch walking on the level and ascending stairs. Gait Posture. 2015; 42(1): 23-6. doi: 10.1016/j. gaitpost.2014.10.024.
Nevitt M, Cummings S, Kidd S, Black D. Risk factors for recurrent nonsyncopal falls. JAMA. 1989; 261: 2663-8. doi: 10.1001/jama.1989.03420180087036.
Feldman F, Chaudhury H. Falls and the physical environment: A review and a new multifactorial fallsrisk conceptual framework. Can J Occup Ther. 2008; 75: 82-95. doi:10.1177/000841740807500204.
Cho KH, Bok SK, Kim YJ, Hwang SL. Effect of lower limb strength on falls and balance of the elderly. Ann Rehabil Med. 2012; 36: 386. doi: 10.5535/ arm.2012.36.3.386.
Melzer I. Postural stability in the elderly: a comparison between fallers and non-fallers. Age Ageing. 2004; 33: 602-7. doi: 10.1093/ageing/afh218.